The summer 2016 uprising was unprecedented in every respect, as it left hospitals across Kashmir flooded with injured and dead. Saima Bhat reports the magnitude of tragedies which also helped Kashmir’s ailing healthcare system look within

As pellets, bullets and teargas shells started to rain on protestors across Kashmir post Burhan Wani’s killing, hospitals turned into new battle zones.
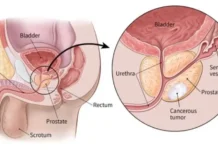
Ophthalmology Trauma Centre

The magnitude of eye injuries was such that doctors managing the crisis termed it ‘record breaking’. As per hospital records more than 1100 civilians’ sustained injuries to either one or both eyes since July 8, 2016. Dr Rashid Maqbool, a consultant at ophthalmology department of SMHS hospital, Srinagar said, ‘the hospital had one operation theatre in use. Two theatres in ophthalmology and one in trauma centre were completely dedicated to eye surgeries.
“On July 09 we performed 56 surgeries against a normal one or two,” said Dr Rasheed. When India’s renowned vetro surgeon Dr S Natarajan landed in Srinagar, he was all praise for local doctors.
The concern he raised was that of the infrastructure and the need of developing an Ophthalmology Trauma Care centre. “It is need of hour in a conflict region like Kashmir,” Dr Natarajan told Kashmir Life in September. He also said that he had been promised by Chief Minister Mehbooba Mufti that a regional ophthalmology trauma centre will be given (which has been approved on papers five years back).
The proposal for establishment of Regional Institute of Ophthalmology (RIO) in Kashmir was approved in 2010, under the centrally sponsored scheme of National Program for Control of Blindness (NPCB). Reportedly GMC submitted a detailed proposal to the state government but since then there is no progress on the proposal. Meanwhile, the same centre on NPCB website lists the RIO location in GMC Jammu.
As per Census 2011, there are 66,448 people with blindness in the state, making it the second highest affecting disability after hearing impairment. And in the new census, the list will have at least 1100 more patients.
Trauma Units

On July 30 evening, Imran (name changed), 25, was part of a peaceful protest rally in Pulwama district which turned violent when government forces reached the spot and youth started pelting stones on them. Retaliating, the forces fired tear gas shells, pellets and bullets, one shell injuring Imran in the back.
“He needed a few more consultations so we had to refer him to Srinagar hospital,” said a doctor who treated him at district hospital Pulwama.
During 2016 crisis, the referrals from peripheral hospitals were reduced to large extent. Out of 9013 total injured patients in district and sub district hospitals across Kashmir, 7484 patients were treated in their districts and only 1529 patients were referred to SMHS hospital, which mostly included eye injuries. Dr Mir Mushtaq, spokesperson Doctor’s association in Kashmir, says that these ‘minimum’ referrals could have been minimized further, if all specialised doctors would have been available at one single hospital. He believes that one single unit of specialized doctors should be in place in every district which eventually will reduce burden on tertiary care hospitals.
=At least 10 trauma centers, six for Kashmir division and four for Jammu, were supposed to come up along the hilly terrain of state but in 2016, all of these unit are still a distant dream. Resultantly the number of deaths in road traffic accidents is also increasing.
A total of 665 people died and 5,923 injured in 4,132 road accidents in Jammu and Kashmir from January-September 2016. In Srinagar, as many as 38 people died and 254 injured in 255 accidents followed. Trauma centers are must in Kashmir. The trauma centre in Bone and Joint hospital too is a semi trauma centre, alleges Dr Imran. “When we receive a patient at B&J, we have to shift him to SMHS hospital for other consultations losing the golden hour, first hour of accident, of a patient,” he said.
Director Health Kashmir, Dr Saleem ur Rehman says that trauma centre involves many things together and confesses that “practically it is not possible to have trauma centers everywhere as it technically means 8 surgeons, 8 orthopedicians, 8 anesthesiologists, 8 technicians, and huge peripheral area.” Although Islamabad district hospital is close to Qazigund trauma centre, the patients prefer to go to Islamabad rather than to trauma centre.
Manpower
Post July 08, Kashmir was put under medical emergency. All staff associated with hospitals were called back on their duties and asked not to leave the station. The doctors in peripheries were on duty for many days together. “We were working continuously, day and night without any rest.” says Dr Ashraf, who works as a consultant in Baramulla district.

A senior doctor in Pattan Sub District Hospital told Kashmir Life “In 420 minutes of being on duty, I have to treat 400 patients. In less than two minutes how can I justify with my profession”. For him, it is important that a doctor talks to his patient and then prescribe medicines.
The Director health also accepts the fact that there is a huge deficit of doctors in the heath sector. “We have manpower which is outdated and against patient: doctor ratio of 1:50,” Dr Saleem says his department is managing the ratio of 1:200
Besides major hospitals, Kashmir division has 12 district hospitals, 55 sub district hospitals, more than 500 PHC’s, 1100 sub centres. “Technically there is no dearth of centres, it is a fact, we have institutions constructed but they are idle”
Diagnostic Equipments

Dr Shaista, who works as a consultant in Kulgam says that in case of emergencies, the need to have proper diagnosis is the only hope to save a patient.
In the last four months, 83 critically injured patients were operated upon in District hospitals, apart from 3680 major/minor surgeries performed upon injured patients. “And not all of the gadgets like CT scans, ECG, ECHO cardiography, digital X rays are available in peripheries,” says Dr Shaista. Regarding diagnostic equipment, Dr Saleem says that they are available everywhere.
Referral System
On August 5 evening, Shazia, 30, a resident of Pulwama district, developed pain in her leg. She was taken to district hospital. Once in casualty ward, she recalls, “It was a mess. I wished to die instead of getting treated. As doctor started examining me on bed, I found around 50 men were looking at me! The doctor was uncomfortable, as well. He became furious and left me unattended” Shazia couldn’t do anything and started weeping.
There was no medical emergency to refer Shazia. “At least 50 percent of the patients who are referred from peripheries are because of the reason that doctors are not able to handle the rush,” says Dr Mir.
Dr Atif Manzoor has a different view. He says that patients are not satisfied as they want to go Srinagar that gives them the satisfaction of being treated at big hospital. He further said that lack of proper referral system is creating more mess.
Dr Manzoor, a retired doctor has served in far flung areas of valley. He said that referrals reduce the efficiency both at the district level and at tertiary care level. “This way we will never develop expertise at district levels. It should not be like passing the buck,” he said.
A few doctors blame security for being weak. So doctors prefer to refer the patient to avoid the consequences.
Blood bank

As the wounds were bleeding, Srinagar’s SMHS hospital transfused 320 blood pints in first ten days to the injured. Besides they also transfused 185 pints of blood including 84 units of plasmas.
The officials in the department of Pathology say that there was no shortage of blood as volunteers were available to donate the blood.
Crisis apart, the infrastructure of blood banks in Kashmir is limited which could prove fatal at times. The stock of rare blood groups in the banks is always often inadequate which leads to the “blood crisis”.
Dr Ajaz lone advises people to donate blood. “The lifespan of an RBC is only 120 days. RBC would anyways get destroyed after this period,” he said and added that government should also intervene to place modern system in place to store blood for longer durations.
In 2016 crisis alone, Dr Saleem says that his hospitals had surplus of supply. “We fortify it from Pulwama and Islamabad to SKIMS hospital, and from Baramulla to JVC and LD hospital.”

Ambulatory Services
Except four ambulances, the vehicles plying with the name of ambulances were all ‘just vehicles’, not fit for transporting patients. The reason is the lack of equipments which provides support to the patient till he reaches to the hospital.
“Our private vehicles were damaged even if we had put Red Cross marks,” said a doctor from Baramulla district hospital, who resides in Islamabad.
Director health services wants to award drivers for their work during crisis. “We have 400 plus ambulances working, 198 ambulances were damaged, but still we didn’t receive one complaint from people.” Dr Saleem says that when nobody could commute, his ambulances ferried doctors from Islamabad to SKIMS Soura, from Baramulla, Islamabad, Bijbehara to SMHS hospital.
During the same period one photo showing an ambulance driver wearing helmet while driving became viral on social networking websites. “My drivers helped doctors, patients to reach their destination and they even escorted a few patients as well. They did excellent work but still they were beaten, they were shot at, they were humiliated,” says Dr Saleem.
But when it comes to the equipments present inside these ambulances, Dr Saleem confesses that they have only four critical care ambulances which he says are stationed at Pampore, Bijbehara, Kreeri hospitals from where critical patients were ferried to hospitals in Srinagar. In extreme cases director health says that they airlifted few patients to SKIMS hospital as well.
“We have been sanctioned 108 ambulances and hopefully we will get them soon,” says Dr Saleem.
Fund allocation
India spends only one percent of its Gross Domestic Product (GDP) on public health, compared to three percent in China and 8.3 percent in the United States.
Out of this one percent GDP, the healthcare in Jammu and Kashmir gets a share of just Rs 100 crore, which includes the tertiary care hospitals as well. “I cannot talk on state health policy on behalf of government,” Dr Saleem ur Rehman said.