by Zubair Lone
To keep its citizens healthy, governments generally use two modalities to provide holistic health services – public health and healthcare. To a common man, the two may appear to mean the same thing. That is not the case though.
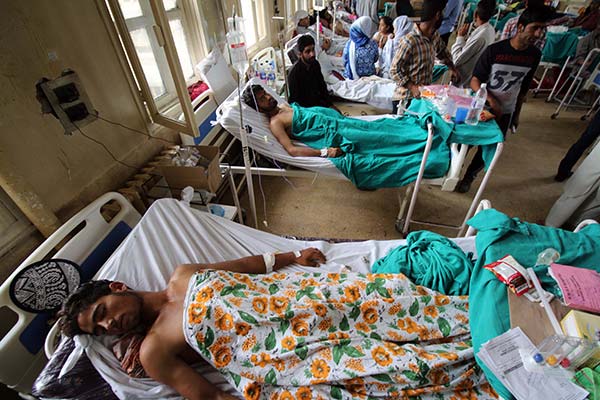
Public health is what a government does to prevent disease and to protect health. While healthcare includes different types of biomedical interventions that are carried out to restore health after an individual falls ill. So, public health is what a government does to protect its already healthy citizens from falling ill and healthcare is all it does to make those who have fallen ill healthy again.
Healthcare, also known as medical services or disease-care, includes visible infrastructure like public health centres, dispensaries, hospitals and clinics. It also includes ensuring biomedical devices, laboratory and diagnostic equipment as well as drugs and medicines. Healthcare is highly labour intensive. In contrast, public health is largely invisible infrastructure, working towards mitigation of social and environmental determinants of diseases and promoting health.

As can be seen, public health and healthcare are, therefore, the two equally essential components of any comprehensive health services system. However, advertently or inadvertently, the Government of India has de-emphasized the public health component through a series of policy decisions since late 1940s and early 1950s; starting with abolishing the public health wing of the earlier British Raj.
Apart from others, these policy decisions largely included a few amalgamations and separations at organizational levels.
First, amalgamation of medical and public health services. The intention behind this was to increase coordination and efficiency. But, it led to the gradual eclipse of public health services by the medical services.
Second, separation of public health engineering (PHE) from health services. This fractured the public health services and disabled the health department from undertaking crucial interventions to promote health at environmental levels.
Third, introduction of single-focus programmes. Such programmes were usually sponsored by international organizations beginning in 1950s with the malaria eradication programme. This was followed by creation of a plethora of such stand-alone vertical projects on tuberculosis, leprosy, polio, AIDS, etc. without the presence of an overarching and integrated public health infrastructure. The failure of such a siloed-approach is highlighted by the fact that even after 60 years of introduction of malaria eradication programme in India, 95% of country’s population is living in “malaria endemic areas” as per the National Vector Borne Disease Control Programme. And India reports more than 1 million cases of malaria annually.
As the central government was busy demolishing the public health component of its health services system, most of the states followed suit.

Jammu & Kashmir is no exception. Medical services have been prioritized and public health services that seek to reduce the population’s exposure to disease, neglected. One of the major reasons, enhancing medical services largely adds visible infrastructure, howsoever ill-planned, under-resourced or over-burdened; and is hence more incentivising in terms of mobilizing vote banks and in terms of greater scope for corruption and fund misappropriations for all and one involved.
A neglected public services and an ill-prioritized medical services are evidenced by the fact that Jammu and Kashmir has the highest number of 2,812 hospitals and health institutions in India, next only to Rajasthan, as per the Health Ministry data and yet not a single hospital in J&K is accredited by the National Accreditation Board of Hospitals (NABH), a constituent board of Quality Council of India. The NABH standards ensure that the clinical aspects and governance aspects of a hospital are process driven and based on clear and transparent policies and protocols. Furthermore, the state population is ever prone to ill-health from communicable diseases and epidemics largely resulting from poor environmental health conditions. Outbreaks of diseases such as hepatitis C, diarrhoea and cholera are commonplace. Likewise, the state also faces a growing threat from non-communicable diseases (NCDs)—cardiovascular disease, cancer, chronic respiratory disease, diabetes, and mental health conditions.

With this in mind, it becomes vital for the central government, in the first place, to re-instate a functional public health infrastructure framework. However, health being a state subject under the Constitution, state governments are also capacitated to take steps to establish an integrated and comprehensive public health infrastructure on their own. In this regard, the Government of J&K can seize the opportunity of taking the lead. It can begin from learning the principles for establishing public health services from Tamil Nadu’s health system.
Notably, the health department of Tamil Nadu has three equally important directorates under the health secretary: the Directorates of Public Health, of Medical Services, and of Medical Education. Moreover, the Directorate of Public Health proactively sustains its initiatives because of a dedicated and a comparatively larger budget. Furthermore, public health service provision in Tamil Nadu is greatly facilitated by legislative and regulatory underpinnings, including a comprehensive public health act. Also, the induction, orientation and training of a well-incentivized staff is towards an administrative and management role rather than a clinical role. They are oriented towards community-wide perspective instead of a patient-specific approach.
All things considered, with a health services system that is broadly based on such principles and then further strengthened by tailoring efforts to suit the local needs, J&K would be able to promote health, respond proactively to avert potential health threats and act quickly and effectively when confronted with diseases, disasters and emergencies through a truly holistic health services system.