SRINAGAR: Even as the Coronavirus (Covid-19) is hitting new territories and storming into newer borders, there is a global consensus that a vaccine will be available only later next year.
USA Today reported that a “usable coronavirus vaccine will probably take 12 to 18 months.” Efforts are underway to produce an RNA vaccine, that may take slightly lesser time but not less than a year. This happened after China decoded the coronavirus’ genetic sequence and made it public on January 10. “That kicked genetic research into high gear around the world, focusing on the virus’ signature protein spikes that circle it like a corona,” the newspaper reported. Oslo based Coalition for Epidemic Preparedness Innovations; a global partnership of companies, public organizations and philanthropic groups is coordinating the development of vaccines. Right now, 79 organisations, 40 biotech companies, 14 pharmaceutical companies and 12 universities and health departments are working to find a cure, according to USA Today.
An Ebola Drug
On compassionate grounds, the British newspaper The Guardian reported that a drug that was part of the initial fight against Ebola is being used in select patients. It, however, is awaiting clinical trials that will take some time. “While awaiting these results, doctors in the US, China and Italy are already using remdesivir on a compassionate basis to treat small numbers of patients with severe Covid-19. The first US patient, a 35-year-old man in Snohomish County, Washington, recovered, but the full trials are needed to assess whether the drug reduces the severity of symptoms and, crucially, mortality rates,” the newspaper reported.
Of the 71325 cases – which are closed, so far, 4382 deaths have taken place that has surged the mortality rate to six per cent. More than 50,000 cases are being tackled with 11 per cent of them in a critical state in 121 countries.
At the same time, however, the world is racing to create some anti-dote and newer researches have resulted in understanding the particular virus better. These inputs could be hugely useful for the people in general and the medical professionals in particular.
John Hopkins Research
Research by scientists at Johns Hopkins Bloomberg School of Public Health said that if a person has not developed symptoms by day 12, he can still be infected, Sky News reported.

“It takes five days for COVID-19 symptoms to show, according to a new major scientific study measuring how patients develop symptoms,” it reported. The research was based on 181 cases from China and elsewhere. “On average those who are ill will show symptoms by day five of the illness, although even if they haven’t developed symptoms by day 12 they could still be spreading the virus.”
The report added: “Current advice for anyone who thinks they could have the disease is to self-isolate for 14 days to avoid spreading the virus to others.”
Professor Justin Lessler, the lead researcher on the study was quoted saying: “Based on our analysis of publicly available data, the current recommendation of 14 days for active monitoring or quarantine is reasonable, although with that period some cases would be missed over the long term.” It added: “It is believed that one in every 100 cases will only show symptoms after the fortnight self-isolation period.”
Added a separate report on the Science.net: “The Johns Hopkins team found that less than 2.5 per cent of those infected would show symptoms within 2.2 days; the estimated median incubation period was 5.1 days; and 97.5 per cent will show symptoms within 11.5 days.”
Wuhan Expert Speaks
News agency Bloomberg talked to Dr Du Bin, director of the intensive care unit at Peking Union Medical College Hospital, who is China’s most respected expert on critical care and was specially flown to Wuhan at the peak of Covid-19 outbreak. He has made some interesting observations.
Du has said that patients with hypertension appear to be at a higher risk of dying from the Coronavirus. “Of a group of 170 patients who died in January in Wuhan — the first wave of casualties caused by a pathogen that’s now raced around the world — nearly half had hypertension,” the report published in Japan Times said.
“From what I was told by other doctors and the data I can see myself, among all the underlying diseases, hypertension is a key dangerous factor,” said Du was quoted saying. “Though there is no research published on that yet, we believe hypertension could be an important factor in causing patients to deteriorate, leading to a bad prognosis.” He added: “We’ll keep an eye on old people and those with high blood pressure. They are the key focus.”
Du has suggested doctors that they should not hesitate to escalate measures for patients facing respiratory distress, as organ failure can set in quickly after. “That means doctors should intervene aggressively with invasive ventilation measures — inserting a tube into a patient’s throat or cutting the throat open to create an airway — when low blood oxygen levels can’t be improved by less invasive measures,” the report said. Respiratory therapists are key help in these procedures.
In Wuhan, there have been instances that people contracted infections even after being discharged and declared fully recovered. He has said that samples taken from different areas of the same patient could test differently depending on where the virus resides. Tool kits in operation have inherent inconsistencies, he has said.
Pregnant Women, Children Safe
What is more interesting is that the Covid-19 has left pregnant women and children untouched despite their seeming physical vulnerability. “From what we known, infected pregnant women do not get into a serious situation with the coronavirus,” Du said. “With influenza, pregnancy is a high-risk factor that can cause severe symptoms and lead to bad outcomes, but not this time.” The report added: “Children infected with the coronavirus also seem to experience only mild symptoms, said Du. He has not seen any child infections deteriorate to a state which requires intensive care.”
Reporting from China for South China Morning Post, Mandy Zuo said the virus has caused “less serious symptoms and lower mortality in women” compared to men, according to two research papers by doctors working in Wuhan.
“In one study of more than 1,000 patients across mainland China, including 37 who died in Wuhan, researchers found that men suffered more severe effects and were more likely to die, accounting for 70 per cent of the death toll, according to a study published on Thursday on medRxiv.org, a preprint server for health sciences.” The report said. Older men with comorbidities, , it said, were “more likely” to get “severe and even fatal respiratory diseases”. The paper was written by researchers from Wuhan Union Hospital and Beijing Tongren Hospital. “An earlier study of 47 patients with coronavirus-induced severe pneumonia found that male patients were more likely to have prior lung disease, develop secondary infections, require complex treatments and experience worse outcomes.”
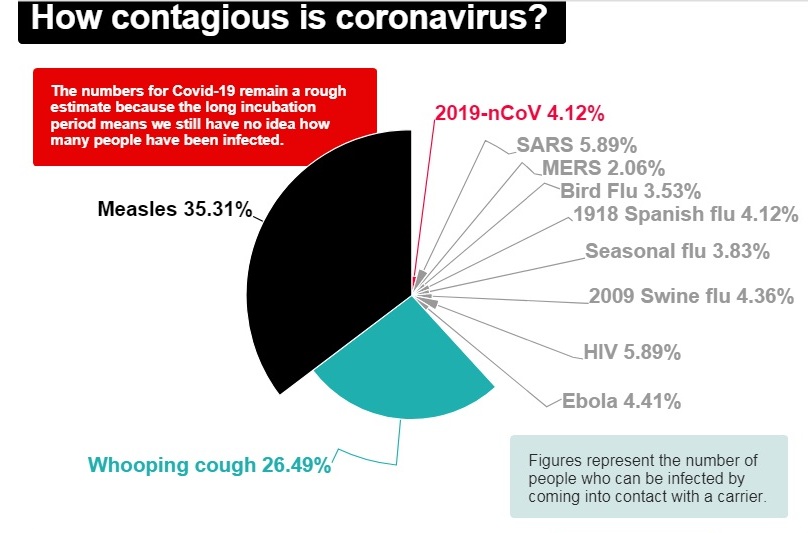
“One of the few mercies of the spreading coronavirus is that it leaves young children virtually untouched, a mystery virologists say may hold vital clues as to how the virus works,” The Washington Post reported. World Health Organisation (WHO) found that only 2.4 per cent of infected were children of whom only 0.2 per cent got critically ill. There has not been the death of any child reported from China.
“Figuring out why children are so unaffected could lead to breakthroughs in understanding how and why the virus sickens and kills other age groups, said Frank Esper, a paediatric infectious disease specialist at Cleveland Clinic Children’s,” the newspaper reported. “Among the questions Esper and others are exploring: Is the severity of infection related to what patients were exposed to previously? Does it have to do with how our immune systems change with age? Or could it be due to pollution damage in the lungs that people accumulate over years?”
Interestingly, the young survived the SARS (2002) and MERS (2012). Coronavirus, scientists say is closer to SARS.
An Infection In Bus
Natalie Brown reported for an Australian news website that an infected patient who uses a bus or a train ends up infecting 14 persons in a day.
“The research, completed by a team of Chinese government epidemiologists, found that a passenger – unaware that they had coronavirus – infected up to 13 other people travelling on the same bus in a matter of hours,” the report said. The virus, the report said, can “linger in the air for at least 30 minutes” and can travel up to 4.5 meters, “further than the distance people have been advised to keep from each other”.
The research in which the researchers have used actual camera footage of the infected and published in Practical Preventive Medicine last week said that in “closed environment with air-conditioning, the transmission distance of the new coronavirus will exceed the commonly recognised safe distance.”
“Lead author of the study Hu Shixiong, who works for the Hunan Provincial Centre for Disease Control and Prevention, said security camera footage showed patient “A” did not interact with others throughout the four-hour ride,” the report said. “Yet, by the time the bus stopped at the next city, the virus had already jumped from “A” to seven other passengers.” By the time the study was finished in mid-February, patient “A” had infected at least 13 people, the report added. By average, the virus is infecting three persons from one carrier. The study has strongly recommended using the face masks especially in buses and places with gatherings.
The virus survival depends on the type of surface and temperature. “On a bus, where common surfaces are made from materials like glass, fabric, metal or plastic, the virus can survive for two to three days,” it said.
Using the same study, the New York Post reported: “Surveillance footage showed that the patient didn’t interact with others throughout the four-hour ride — but a couple of the people who became infected were sitting as far as six rows away, or about 15 feet.”
Avoid Ignoring Gastro Angle
A study published in The Lancet that examined 99 of the earliest cases of the 2019 coronavirus in Wuhan suggest that some patients reported diarrhoea, nausea, vomiting and abdominal discomfort. The same situation was found in the US’s first victim of the virus.
“In this paper that focused on gastrointestinal symptoms, it is clear that the virus doesn’t only bind to lung tissue but also the tissue of the colon, upper oesophagus and liver amongst others,” a news report said. “This means that medical professionals might be making a greater effort to spot digestive issues for earlier detection, diagnosis and isolation of the new coronavirus. The way the virus adheres to cells and which enzymes are activated in the process can also help with a potential treatment or vaccine.”
Vitamin C Unhelpful
Though the Vitamin-C intake is shortening marginally the recovery from the common cold, the medical community believes that it is unhelpful in Coronavirus.
Note that no evidence suggests that other so-called immune-boosting supplements — such as zinc, green tea or Echinacea — help to prevent SARS-CoV-2 infections, Dr Mark Mulligan, division director of the infectious diseases and vaccine centre at NYU Langone Medical Center, told New York Times Parenting. “I do not recommend spending money on supplements for this purpose,” Mulligan said.
“But vitamin C supplements don’t ward off the common cold in most people, and there’s even less evidence that they grant immunity against SARS-CoV-2, the virus that causes COVID-19,” Nicoletta Lanese reported in Live Science.
Virus Shedding
“People who contract the novel coronavirus emit high amounts of virus very early on in their infection,” American Stat News reported on basis of a German study, the first non-China study on the issue, explaining the rapid and efficient way in which the virus has spread around the world. The study carried out by scientists in Berlin and Munich envisaged monitoring the viral shedding of nine infected people and they tried to grow viruses from sputum, blood, urine, and stool samples were taken from the patients.
“Importantly, the scientists could not grow viruses from throat swabs or sputum specimens after day 8 of illness from people who had mild infections,” the report said. It quoted authors saying: “Based on the present findings, early discharge with ensuing home isolation could be chosen for patients who are beyond day 10 of symptoms with less than 100,000 viral RNA copies per ml of sputum,” insisting that at that point “there is a little residual risk of infectivity, based on cell culture.”
“The researchers found very high levels of virus emitted from the throat of patients from the earliest point in their illness —when people are generally still going about their daily routines,” it said. “Viral shedding dropped after day 5 in all but two of the patients, who had a more serious illness. The two, who developed early signs of pneumonia, continued to shed high levels of virus from the throat until about day 10 or 11.”
The finding, the report said is “a marked departure” from the SARS in which “peak shedding of virus occurred later when the virus had moved into the deep lungs.” It added: “The scientists said at peak shedding, people with Covid-19 are emitting more than 1,000 times more virus than was emitted during peak shedding of SARS infection, a fact that likely explains the rapid spread of the virus.” The German researchers found high levels of viral fragments in 13 stool samples from four patients in their study, but they were unable to grow virus from any of them.















