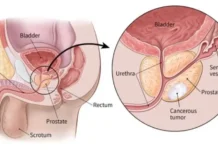
Rising early-onset colorectal cancer in Kashmir, late-stage detection, low screening uptake, and social and financial barriers underscore the urgent need for systematic colonoscopy-based prevention strategies, reports Afreen Ashraf
On a cold Wednesday winter morning, Gulshan Akhtar, 48, was preparing for an angiography scheduled for the next evening. Hours before the procedure, however, doctors ordered one final test, an iron profile, after noticing her persistently low haemoglobin levels.
When the reports arrived, her husband was called in and informed that her haemoglobin was critically low. The doctors informed the family that angiography could not be performed at that stage. Given her fragile condition, even minimal blood loss posed a life-threatening risk. They advised shifting her to the general medicine ward, completing discharge formalities, and returning after three months once the underlying condition had been thoroughly assessed and stabilised.
Subsequently, in the general ward, further investigations began. Repeated tests suggested that something was wrong in her gastrointestinal tract, possibly internal bleeding. A gastroenterologist advised her endoscopy. Even it revealed nothing concerning. The doctors then recommended another procedure, one that was entirely unfamiliar to her, colonoscopy.
Confused and anxious, Gulshan began inquiring about it and eventually learned more about the procedure from an acquaintance. She hesitated. She was told that it was an awkward procedure. She asked the doctor if there was any alternative. But the answer was firm.
“If we don’t evaluate you completely,” the doctor explained, “and if the source of bleeding is in the colon, it will not reveal itself any other way.”
As the date drew closer, her anxiety deepened. She began to anticipate humiliation, replaying every conceivable worst-case scenario in her mind.
Finally, the day arrived. She recalls feeling brief dizziness and a slight pricking sensation during the procedure. Later, she learned that three polyps near her colon had been detected and removed immediately. Biopsy samples were sent for further testing.
At first, she struggled to comprehend what had happened. When she stepped out of the procedure room and saw her family waiting, fear overtook her. “I thought they had found something terrible,” she recalls. “I kept thinking, maybe this is the end.”
She was later reassured and told what polyps are. However, she was not informed that polyps can sometimes turn cancerous, as the doctors wanted to avoid causing her further panic.
Until the biopsy report arrived, anxiety loomed over the family. Everyone waited to learn what had been growing inside her. When the results finally came, they brought immense relief; the polyps were benign.
Nothing Unique
Gulshan’s case is not unique. Across Kashmir, doctors are noticing a worrying trend: Kashmir faces a growing colorectal cancer threat.
Across Kashmir, the incidence of colorectal cancer is estimated at around 16.8 per cent, making it the second most common cancer in the region after stomach cancer. Gastrointestinal malignancies, including CRC, account for more than one-third of all cancer cases, highlighting the heavy burden of digestive tract cancers in Jammu and Kashmir.
According to a 2022 study published in The Lancet Oncology, only 71.6 per cent of adults aged 50 to 75 underwent appropriate colorectal cancer screening in 2020. Screening programmes in most Western countries traditionally begin at age 50, as colorectal cancer (CRC) has long been considered a disease of older adults. Yet in Kashmir, emerging data suggest a different pattern.
Nearly 19.25 per cent of all diagnosed colorectal cancer patients in the region are below the age of 35, according to data from Sher-i-Kashmir Institute of Medical Sciences and Government Medical College Srinagar. A growing concern is the rising number of patients under 50 who do not follow routine screening guidelines.
In Kashmir, colorectal cancer is emerging at a comparatively younger age. Most cases are reported between 56 and 65 years (24.2 per cent), nearly a decade earlier than typical diagnoses in the United States and Europe. Hospital-based data analysis of 1,598 cancer patients between 2006 and 2012 further highlights its growing significance. Among men, colorectal cancer accounted for 16.4 per cent of cases, while among women, it ranked as the most common cancer at 16.8 per cent. Although global population studies have traditionally shown a male predominance in colorectal cancer, the data from Kashmir suggest a substantial burden among both genders, indicating that the disease is not only affecting people earlier but also impacting women at notable rates.
Danger of Late Detection
Nearly half, 49.8 per cent, are detected at Stage III, and 5.5 per cent at Stage IV, meaning the cancer has already spread by the time it is found. Only a small number are diagnosed early, at Stage I or II, when treatment is most successful.
“Colorectal cancer does not develop overnight,” Dr Riya,z a gastroenterologist at Nora hospital, said. “ There is a window for prevention, but people are not coming forward in time.” Doctors in tertiary hospitals in Kashmir report seeing patients with colorectal cancer at advanced stages
The data have prompted serious concern among clinicians. “With the shift towards younger age groups that we are observing in Kashmir, it may be time to reassess the recommended age for initiating screening, particularly for high-risk individuals,” says Dr Parra.
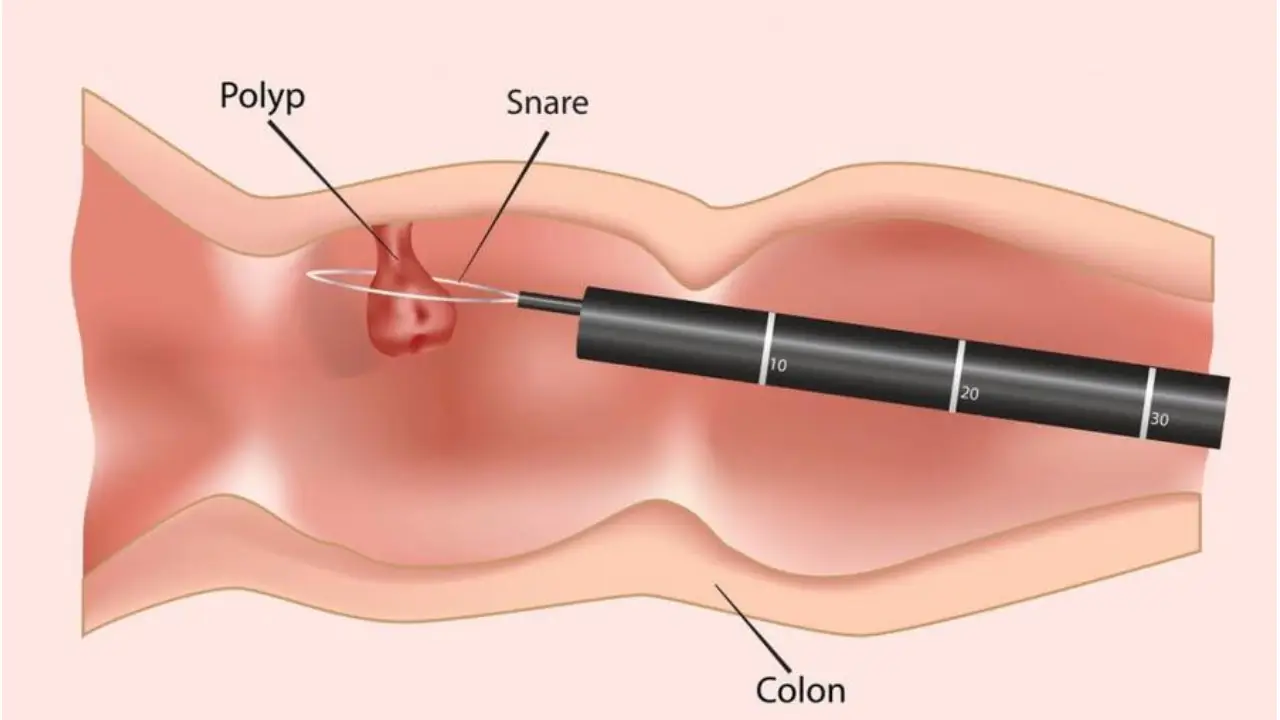
Colonoscopy remains the primary tool for detecting and preventing colorectal cancer, allowing doctors to identify and remove precancerous polyps. Yet, despite its proven effectiveness, a significant number of people do not undergo routine screening.
| State of Cancer in Jammu and Kashmir and Ladakh | ||||||||||||
| State | Type | 2014 | 2015 | 2016 | 2017 | 2018 | 2019 | 2020 | 2021 | 2022 | 2023 | 2024 |
| Jammu and Kashmir | Overall | 14115 | 14864 | 15652 | 16480 | 17351 | 12396 | 12726 | 13060 | 13395 | 13744 | 14112 |
| Ladakh | 279 | 286 | 294 | 302 | 309 | 318 | ||||||
| Jammu and Kashmir | Breast CA | 569 | 586 | 603 | 619 | 638 | 656 | 674 | 694 | 712 | 732 | |
| Ladakh | 12 | 12 | 12 | 13 | 13 | 13 | 14 | 14 | 15 | 15 | ||
| Jammu and Kashmir | Cervical | 233 | 241 | 248 | 256 | 261 | 269 | 278 | 285 | 293 | 301 | |
| Ladakh | 6 | 6 | 6 | 6 | 7 | 7 | 7 | 7 | 7 | 7 | ||
| Source: Government Data shared in Lok Sabha | ||||||||||||
A Test, A Procedure
“The encouraging aspect is that colorectal cancer is among the most preventable cancers,” Dr Reyaz A Parra, a gastroenterologist at Noora Hospital. “With age and family-based screening, small polyps can be detected early, during colonoscopy, thereby preventing cancer.”
Small growths called polyps often sprout from inside the colon without causing any symptoms. Over time, some of these polyps can turn into cancer. During a colonoscopy, doctors can detect and remove these polyps immediately, preventing cancer before it starts.
“Colonoscopy is not just a test, it is an opportunity to prevent cancer before it starts,” Dr Reyaz said. “Colonoscopy is a straightforward test that allows direct visualisation of the intestines using a thin, flexible tube with a camera.”
The procedure is often misunderstood, with many assuming it is painful or inherently risky. In reality, it is generally safe, performed under sedation, and associated with minimal discomfort. The examination usually lasts between 20 and 40 minutes, and patients are discharged the same day.
The procedure enables physicians to identify ulcers, internal bleeding, inflammatory bowel disease, and early-stage colorectal cancer, facilitating timely diagnosis and intervention.
By the time symptoms like bleeding, anaemia, weight loss, or persistent bowel changes appear and alert the physician, the disease may already be advanced. Yet discussions around bowel health are still limited in many communities, including Kashmir, leading to delays in screening.
Doctors have a consensus on one thing: “If proper screening protocols are followed based on age and family history, small polyps can be detected early and removed through colonoscopy, preventing cancer.”
Screening, Whom?
Doctors believe Kashmir may be more vulnerable to colorectal cancer due to a combination of dietary habits and lifestyle changes. Traditional foods include noon chai, pickled vegetables, smoked meats, and high consumption of red meat. While these foods are part of cultural identity, regular intake of heavily salted and preserved items may increase the risk of gastrointestinal problems over time.
At the same time, dietary fibre intake from fresh fruits, vegetables, and whole grains remains insufficient for many. A sedentary lifestyle has further compounded the risk. Delayed health-seeking behaviour is another critical factor. Early warning signs, such as mild rectal bleeding or subtle changes in bowel habits, are often ignored due to hesitation, stigma, or lack of awareness. Consequently, conditions that progress gradually, including colorectal cancer, frequently go undetected until they have advanced to later stages.
Doctors advise that, ideally, every individual above 40 years of age should undergo at least one colonoscopy, even in the absence of symptoms or a family history of colorectal cancer.
However, certain inherited conditions, collectively termed familial colorectal cancer syndromes, necessitate much earlier surveillance. One such disorder is Familial adenomatous polyposis, in which the colon may develop hundreds or even thousands of polyps, many carrying a high malignant potential. In these high-risk cases, screening can begin in childhood.
Similarly, individuals with a first-degree relative diagnosed with colorectal cancer are generally advised to undergo a colonoscopy 10 years earlier than the standard recommended age, or even sooner, depending on clinical assessment. While sporadic polyps typically take 10–15 years to progress to cancer, this interval is considerably shorter in syndromic families, underscoring the importance of early and regular screening for effective prevention.
Health Care Infrastructure
In Kashmir, advanced endoscopic services are concentrated primarily in Srinagar, with Sher-i-Kashmir Institute of Medical Sciences serving as the valley’s main tertiary referral centre and high-volume training hub. Long waiting lists in public hospitals have led to a parallel expansion in the private sector, including Noora Hospital, Ramzaan Hospital, Paras Hospital Srinagar and Wellcare Medical Institute, which now play a critical role in providing diagnostic and therapeutic colonoscopies.
Despite this availability, screening coverage remains low. According to global cancer data, regular screening significantly reduces both incidence and mortality of colorectal cancer by detecting precancerous lesions early, yet uptake remains inconsistent due to limited organised programmes.
“In many countries, routine screening for gastrointestinal malignancies is part of national health programmes and is covered by insurance,” Dr Reyaz Ahmad Para explained. “Unfortunately, we are still lacking such screening systems here. The state does not finance these screenings.”
Barriers to Screening
In Kashmir, colorectal cancer is not merely a clinical concern; its trajectory is shaped by entrenched beliefs, financial constraints, and social norms that collectively delay timely screening. The most immediate barrier is a lack of awareness.
Symptoms such as rectal bleeding or altered bowel habits are frequently dismissed as minor ailments, often attributed to “piles”, resulting in late-stage presentation. Many individuals resort to home remedies or over-the-counter treatments instead of seeking medical evaluation. By the time professional care is pursued, the disease may have advanced considerably, mirroring global trends where colorectal cancer is commonly diagnosed only after symptoms become pronounced.
Economic factors further compound the problem. Although government hospitals offer subsidised services, extended waiting periods often compel patients to seek care in private facilities, where colonoscopy costs can range from Rs 6,000 to Rs 20,000. If malignancy is confirmed, comprehensive treatment may cost between Rs 1.5 lakh and Rs 6.5 lakh, an overwhelming expense for many households.
Cultural hesitation adds another layer of delay. “The day I went to book my appointment, I looked into the room and saw a procedure being performed on a woman by a male doctor,” Gulshan recalls. “From that moment, my hesitation only deepened. I felt ashamed at the thought of being partially undressed in front of a male doctor.”
For many women, embarrassment and anxiety surrounding bowel health, still a largely unspoken subject, discourage timely screening, further postponing diagnosis and care.
A Lesson.
Gulshan had not sought care for polyps; she had come to the hospital for a cardiac evaluation. In the same facility, 52-year-old Aijaz Ahmed presented with severe abdominal pain initially suspected to be appendicitis. A subsequent colonoscopy, however, revealed inflammatory bowel disease. Neither patient had anticipated a gastrointestinal diagnosis.
Both discoveries were incidental. Their experiences illustrate a broader clinical reality: many gastrointestinal disorders, including precancerous lesions and malignancies, remain asymptomatic for years.
Patients often feel entirely well until a complication arises or an unrelated investigation prompts further evaluation. This silent progression underscores the insidious nature of early colorectal disease and reinforces the importance of proactive screening, a principle consistently supported by global data showing significantly improved survival with early detection.
Doctors Appeal
Gulshan and Aijaz were fortunate. Their conditions were identified before irreversible damage occurred. But many others never reach that point of timely diagnosis. How many continue to dismiss rectal bleeding as piles? How many defer screening because of cost, social discomfort, or the absence of overt symptoms?
In a region where colorectal cancer is increasingly affecting younger adults, a symptom-driven approach may no longer be adequate. Colonoscopy is not simply a diagnostic intervention; it is a preventive strategy capable of interrupting disease progression before malignancy develops.
Dr Reyaz Ahmad Para emphasised the urgency. “I would strongly like to draw attention to colorectal screening. People should be made aware of its importance,” he said. “Whenever a patient presents with symptoms related to the lower gastrointestinal tract, we always advise a colonoscopy.”
Addressing concerns about heredity, he added, “Having a family history does increase genetic risk, but it does not mean cancer is unavoidable. That is exactly why I emphasise screening.”
Reframing colonoscopy, not as a painful or embarrassing procedure, but as a scientifically validated preventive measure, is essential to reducing the disease burden. Awareness, timely clinical evaluation, and adherence to recommended screening protocols collectively offer the most effective defence.
The distinction is stark: detect early and prevent, or detect late and treat. As Dr Reyaz Ahmad Para underscores, timely screening can prevent cancer.