Dr Afshan Iqbal, a senior gynaecologist, speaks to Syed Shadab Ali Gilani about rising infertility concerns, PCOS, C-sections and maternal health, offering evidence-based guidance for couples. Afreen Ashraf prepared the conversation for publication.
KASHMIR LIFE (KL): People are talking about infertility. What are the main reasons for the high infertility rates in Kashmir?
DR AFSHSAN IQBAL (AI): It is important to first define who is considered infertile and what constitutes an infertile couple.
In clinical practice, fertility can only be assessed after understanding a couple’s married life, the duration of marriage, and whether they are in a regular physical relationship. Medically, infertility is defined as when a couple has been trying to conceive for more than one year without success.
The timing of investigations, however, depends largely on age and health status. For women under 30–35 years with no medical issues, evaluation usually begins after one year. But if there are co-morbidities like hypertension, diabetes, or other chronic illnesses, investigations should start earlier, around six months.
Naturally, about 80 per cent of couples conceive within the first year, and nearly half of the remaining conceive in the second year. Overall, almost 90 per cent achieve pregnancy within two years. Therefore, infertility rates should only be estimated after applying these criteria.
In Kashmir, marriage patterns are changing, with early marriages becoming common again. Yet many young couples begin worrying about pregnancy immediately after marriage. This often leads to unnecessary stress and, at times, overtreatment. Treatment should be based on age and medical need, not anxiety.
Infertility is a global issue, but the approach must be rational and stepwise. Couples need proper counselling about what to expect, when conception is likely, and when medical intervention is actually required. Excessive stress itself can reduce the chances of pregnancy.
For women under 35 years with a normal weight and no health problems, it is advisable to wait at least one year before seeking treatment. Young couples should focus on their early married life without pressure, while avoiding contraceptives.
Counselling both partners is essential, as infertility is not solely a female issue. Nearly 30 per cent of cases involve male factors. Therefore, both partners must be evaluated and treated together when needed.
Management follows a structured approach: initial investigations, followed by basic treatment, and then advanced options such as laparoscopy or IVF if necessary. Unfortunately, due to a lack of awareness, some couples switch doctors when advised advanced treatment, which disrupts continuity of care. Changing doctors does not improve outcomes; systematic treatment does.
It is also common to see couples continuing the same basic medications for six or seven years without reassessment. This is ineffective, as fertility declines with age. Women above 40 face reduced conception rates and higher risks of miscarriage.
KL: Do these medicines have side effects?
AI: We use globally prescribed medicines. We do not give medicines with significant side effects, especially because some patients need to take them for a longer period of time.
KL: How much does stress impact pregnancy?
AI: Stress significantly reduces fertility rates, which is why counselling plays a crucial role in infertility care. In many countries outside India, dedicated counselling rooms are an integral part of fertility centres.
Even when such couples conceive, they often experience high levels of anxiety throughout pregnancy. Routine symptoms like nausea or vomiting can cause excessive worry, and people are more prone to emotional distress and depression.
For this reason, I advise couples, especially in the first year of marriage, not to panic unnecessarily. Medical help should be sought only if there is a genuine health concern. Otherwise, young and healthy couples do not need to rush into medication. Waiting for at least one to one-and-a-half years is both safe and reasonable.
We frequently observe that couples who discontinue long-term medications sometimes conceive naturally, simply because their stress levels decrease. This clearly highlights the strong link between anxiety, stress, and reduced fertility.

KL: In Kashmir, the rate of PCOD and PCOS is quite high. What exactly are these conditions in layman’s language?
AI: PCOS and PCOD are very common conditions, particularly in Kashmir, with almost 30-35 per cent of women affected by this problem.
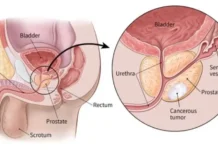
PCOS is diagnosed based on three main criteria. The first is the characteristic appearance of the ovaries on ultrasound. The second is irregular or infrequent menstrual cycles. The third is clinical or biochemical evidence of excess male hormones, known as hyperandrogenism, which may present as facial hair growth, acne, or hair thinning. If a woman meets any two of these three criteria, she can be diagnosed with PCOS.
However, the approach is different in adolescents. During the teenage years, irregular periods are common and part of normal hormonal maturation. Therefore, to avoid overdiagnosis and unnecessary treatment, all three criteria must be present before labelling an adolescent girl with PCOS. After the age of 20, the diagnosis can be made if any two of the three criteria are present.
KL: What are the primary reasons for developing PCOS?
AI: PCOS develops due to multiple interacting factors. Over the past 15 years, lifestyle changes have played a significant role in its rising prevalence.
There is a clear genetic predisposition, and populations in South-East Asia are generally more susceptible. However, the condition was less commonly seen in earlier decades because dietary patterns were simpler and daily life involved more physical activity. Today, higher calorie and nutrient intake combined with a sedentary lifestyle has led to weight gain and metabolic changes. As a result, the underlying genetic tendency toward PCOS is being expressed more frequently.
KL: How can one protect oneself from these problems?
AI: Maintaining a healthy lifestyle is important not only for PCOS but for overall well-being. Once a woman is diagnosed with PCOS, keeping a healthy body mass index (BMI) becomes especially important. BMI is calculated as weight in kilograms divided by height in metres squared, and the normal range is ideally between 19 and less than 25. Staying within this range helps prevent several metabolic and hormonal disorders.
Treatment depends on the patient’s age and symptoms. For instance, if a teenage girl meets the diagnostic criteria for PCOS, counselling is the first step. Specific treatment is then tailored to her concerns, such as acne, hair loss, or excessive hair growth.
In general, all patients are advised to avoid junk food, maintain an ideal body weight, and adopt healthier habits. A large number of women seen in outpatient clinics are married patients with PCOS who also face infertility. PCOS often leads to irregular menstrual cycles due to poor or absent ovulation, which can eventually affect fertility.
This is why awareness about PCOS is essential. What may appear to be a minor menstrual issue can later contribute to infertility. Maintaining a healthy BMI is critical, as medical treatment is far more effective when weight is under control.
Weight reduction, balanced nutrition, and regular exercise play a key role in both preventing and managing this condition.
KL: Can PCOS occur in girls with normal body weight?
AI: Yes, PCOS can affect girls of any body weight. In fact, when a girl with normal or low weight is diagnosed with PCOS, management can sometimes be more challenging because the hormonal profile differs, and treatment protocols need to be adjusted accordingly.
In overweight or obese patients, medications alone often produce limited results. This is why weight management is strongly emphasised, as it is one of the most controllable factors. Without weight reduction, some patients may eventually require advanced treatments such as IVF to conceive. Even when pregnancy occurs, they face higher risks of complications like diabetes and high blood pressure.
KL: What are the primary reasons for premature births?
AI: A birth is termed preterm when a baby is delivered before 37 completed weeks of pregnancy.
Preterm birth generally occurs due to two major causes: the early onset of labour or premature rupture of membranes. In some cases, reduced blood flow to the baby due to placental dysfunction can also necessitate early delivery.
The causes vary. A previous history of preterm delivery increases the risk in subsequent pregnancies. Structural factors, such as a small or abnormal uterine cavity, may also contribute. Multiple pregnancies, including twins or triplets, place additional strain on the uterus and raise the likelihood of early delivery. Excess amniotic fluid is another known risk factor. Obesity and conditions such as diabetes further increase vulnerability.
Placental issues may be more common with advancing maternal age, particularly around 40 years, when placental function may be weaker. However, age alone is not the only factor. Chronic hypertension, autoimmune disorders, and other medical conditions can also play a significant role.
KL: In Kashmir, C-section deliveries have increased. Why?
AI: The rate of Caesarean section deliveries has increased not only in Jammu and Kashmir but across the world. In the current scenario, it is important to understand that this rise cannot be attributed solely to doctors. Often, when a C-section is advised, couples tend to blame the doctor, particularly in the private sector. However, the trend is similar in large tertiary hospitals as well, where dozens of C-sections may be performed in a single night. This clearly indicates that the increase is driven by medical need rather than financial motives.
One major reason is the growing preference to prioritise safety, both for doctors and patients. While C-sections are generally safe and lifesaving when indicated, they are not without risks. They carry potential complications and can affect future pregnancies and surgeries.
For example, women with a previous C-section may develop a scar pregnancy. They are also at higher risk of placental complications such as placenta previa and placenta accreta spectrum. Many of these issues arise as long-term consequences of a prior Caesarean delivery.
KL: If the first baby is delivered through a C-section, is there a chance of a normal delivery next time?
AI: Yes, there is a definite possibility. Globally, the success rate of a normal delivery after a previous C-section, known as VBAC (vaginal birth after Caesarean), is around 70 to 75 per cent, provided all medical criteria are carefully met. However, such cases require strict monitoring and continuous one-to-one care during labour. In regions like Kashmir, this can be challenging due to heavy patient loads and limited resources.
Another concern with C-sections is that babies may sometimes be delivered earlier than necessary, without adequate time for natural physiological adaptation. This can increase the risk of breathing difficulties in newborns. As with any surgery, there is also a higher risk of infection and other operative complications.
Patient preference also plays a role. Some women opt for a C-section to avoid the pain of labour, and attendants may lack the patience required for a normal delivery, which can take 12 to 16 hours. Although both normal delivery and C-section carry risks, complications arising from normal labour are often less acceptable to families.
Therefore, the responsibility is shared. Some patients are reluctant to attempt normal delivery, while doctors, prioritising maternal and foetal safety, may choose the more controlled option of a C-section. With smaller family sizes becoming the norm, many couples prefer what they perceive to be the safest approach. As a result, the rise in C-sections cannot be attributed to any single factor but is influenced by multiple medical and social considerations.
KL: As a doctor, which type of delivery do you suggest?
AI: For a first pregnancy with no complications, I would definitely suggest a normal delivery. While the immediate difference between the two may not seem very large, normal delivery has fewer effects on future pregnancies compared to a C-section.
KL: So, if there are no complications, should patients wait, and is counselling necessary?
AI: Yes, counselling is very important. However, in the government sector, the patient load is extremely high, which limits the time available for detailed counselling. As a result, many women are asked to return closer to their due date, and some may present late or already in labour without adequate preparation.
In the private sector, we often see second- or third-time mothers. Among first-time mothers, preferences vary; some request a planned delivery date to avoid labour pain, while others prefer to wait for a normal delivery. In such situations, we provide proper counselling, explain the risks and benefits of both options, and proceed according to the patient’s choice, provided there are no medical complications.
KL: What are the major causes of stress during pregnancy and after pregnancy?
AI: The overall rate of stress, depression, and anxiety in Kashmir is quite high. Pregnancy itself is stressful due to hormonal imbalance. Women often become irritable, and in some cases, a history of depression gets triggered. During this phase, a pregnant woman cannot manage everything on her own, so family support becomes very important.
I recently witnessed a case where a woman felt continuous nausea just because of making an omelette for her husband. In such situations, the partner needs to understand and cooperate. These issues cannot always be treated with medicines alone.
Women already on antidepressants should continue their medication after proper consultation with their doctor. Stopping treatment abruptly can worsen symptoms and increase the risk of complications.
Postpartum depression is fairly common after delivery, and women with a prior psychiatric history are at significantly higher risk. Patients who have been on antidepressants or antipsychotics may experience greater emotional or psychological difficulties in the postpartum period.
Early recognition is crucial. Treatment depends on the severity of symptoms and may include medication, counselling, or a combination of both.
Equally important is strong family support. The hormonal changes after childbirth can cause mood swings, irritability, and emotional distress, which should be understood with empathy rather than criticism. Families should actively assist with newborn care, helping at night, sharing responsibilities during the day, and ensuring the mother gets adequate rest.
KL: During pregnancy, what safety measures should be taken?
AI: Once a couple conceives, the first step is to assess the mother’s age, as this helps categorise the pregnancy as high-risk or low-risk. Any underlying medical conditions such as hypertension or diabetes, are screened early, making the first antenatal visit particularly important. In low-risk cases, there is generally little cause for concern.
Pre-pregnancy or early pregnancy folic acid supplementation is advised. An initial ultrasound is usually performed at six to seven weeks to confirm viability and dating. The first-trimester screening or anomaly scan is then done between 11 and 13 weeks.
For symptoms like nausea and vomiting, medications may be prescribed if necessary. A balanced diet rich in fruits and fresh foods is recommended. However, some women experience gastric discomfort in early pregnancy and may not tolerate certain foods, so force-feeding should be avoided. During the first trimester, it is better to eat small, preferred meals while ensuring adequate hydration, as the risk of urinary infections is higher.
Fat and sugar intake should be limited. Pregnancy requires only about 300 extra calories per day above the normal diet. Light exercise, around three times a week, is also encouraged, as it supports both physical and mental well-being.
KL: Till which month can a pregnant woman continue working?
AI: This largely depends on her medical condition and whether the pregnancy is classified as high-risk or low-risk. If a woman experiences symptoms such as bleeding, abdominal pain, or other complications, she is usually advised to limit travel and avoid work. In conditions like recurrent placental bleeding, risk of preterm labour, or after procedures such as cervical cerclage, adequate rest becomes essential.
However, in low-risk pregnancies, there is generally no restriction on working. Many women safely continue their jobs until 35–36 weeks and then take maternity leave. Some may choose to rest earlier if they feel fatigued. Pregnancy is a normal physiological process and, in uncomplicated cases, does not automatically require bed rest.
KL: What are the dos and don’ts for a normal pregnancy?
AI: If the pregnancy is normal, the woman should continue living normally. Only activities with a risk of falling should be avoided. Excessive climbing up and down should also be avoided. We cannot restrict movement simply because of pregnancy. Otherwise, a large portion of the population would become bedridden unnecessarily.