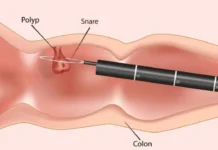
Quietly but surely, prostate cancer is becoming one of Kashmir’s most urgent health crises, and most men do not know they have it until it may be too late, reports Asrar Syeed
Cancer has arrived in Jammu and Kashmir with a persistence that health professionals can no longer speak of in hushed tones. Official data reveal that an average of 38 patients are diagnosed with some form of cancer every single day. This figure has alarmed clinicians and unsettled lawmakers. It has also forced the public into an uncomfortable reckoning with a disease long associated with distant cities and foreign statistics.
In the past five years alone, the total number of registered cancer cases has reached 67,037. Its scale has prompted some to reach for extraordinary comparisons. “The disease is killing people faster than the long-pending conflict,” one lawmaker observed, a statement that, however stark, speaks to the depth of public alarm.
Among the most common cancers recorded are those of the lung, breast, oral cavity, cervix, pancreas, and prostate. It is this last one, prostate cancer, that has been drawing particular concern from urologists and oncologists working across Kashmir.
Once a relatively rare diagnosis, it has been climbing steadily up the charts, not just in Kashmir but across India, where it now ranks as the third most common cancer among men. A disease once considered a concern of the elderly and the affluent West has quietly taken up residence in Kashmir’s clinics and hospital wards.
What the Prostate Fails
To understand prostate cancer, it helps to understand the gland itself. The prostate is small, roughly the size of a walnut, and sits below the urinary bladder, directly in front of the rectum. It encircles the urethra, the tube that carries both urine and semen out of the body. Its primary function is reproductive: the prostate produces the seminal fluid that nourishes and transports sperm.
Prostate cancer begins when normal cells in the gland start to grow abnormally and uncontrollably. The most common form is adenocarcinoma, which accounts for about 95 per cent of cases worldwide. In this type, the cancer originates in the gland cells that produce seminal fluid.
When these cells develop genetic mutations, they begin multiplying without restraint, forming tumours that, left unchecked, can spread far beyond the gland itself.
The disease has four recognised stages. In the first, the cancer is small and entirely confined to the prostate. By the second, the tumour has grown but remains within the gland. The third stage sees the cancer breach the prostate’s outer capsule. By the fourth stage, the stage at which a devastating proportion of Indian patients are first diagnosed, the cancer has spread to the bones, bladder, rectum, or lymph nodes. Recovery at this stage is rare. The window in which the disease is most treatable is also, tragically, the window in which it is least likely to be detected.
Felt Nothing
Peer Mohammad Fayaz had no reason to be worried. Throughout his adult life, he had experienced no urinary complaints, taken no medication for any related condition, and felt nothing that might have prompted concern. There were, he said, “completely no symptoms” that would have led him to seek a PSA test or consult a doctor.
Then, in October 2025, things changed.
“I started showing symptoms like weak urination, slight pain in the pelvic region and other urinary tract ailments,” he recalled. He consulted a doctor. An MRI was ordered, which initially returned no clear result. A biopsy followed, and it showed unambiguous signs of prostate cancer. A subsequent PET scan confirmed the diagnosis.
Fayaz was operated on at SKIMS, the Sher-i-Kashmir Institute of Medical Sciences, Kashmir’s premier multi-speciality hospital.
He was one of the fortunate ones: his cancer was caught before it reached the terminal stage. But his experience illuminates a pattern that doctors across Kashmir describe with growing frustration: men presenting only after symptoms become impossible to ignore, by which point the disease has often advanced considerably.
Fayaz himself now speaks candidly about what his silence nearly cost him. “Lack of awareness among men can become fatal,” he said. “Someone can lose life due to late treatment.”
A Crisis of Awareness
The problem, doctors agree, is not simply medical. It is cultural.
“Lack of awareness and proper surveillance are the main reasons behind increased mortality rates across India,” said Dr Yawar, a urologist at SKIMS. “Early detection and treatment are paramount in decreasing the mortality rates.”
Across India, urology experts have long flagged the striking absence of awareness among men regarding their urological health. Unlike women, who are increasingly familiar with the concept of routine gynaecological screening, most men have little understanding of what the prostate does, when it can go wrong, or what symptoms warrant investigation. The PSA, Prostate Specific Antigen, test is a straightforward blood test capable of flagging potential prostate abnormalities at an early stage. Yet most men in Kashmir, and across India, have never taken one.
This is compounded by the absence of a national screening programme. India has no population-wide PSA testing initiative, partly due to legitimate concerns about over-diagnosis, the possibility that widespread screening might identify slow-growing cancers that would never cause harm, leading to unnecessary treatment. But the consequence of this caution is visible in the data.
“Prostate cancer is among the top three causes of cancer in men and is a cancer of age above 60 years,” said Dr Saqib Ahmad Shah, a consultant oncologist at Paras Hospital who holds a DM in Oncology. “Figures are alarming as cases are increasing. The reason is that 50 per cent of cases in India are diagnosed at stage four, compared to the West, where 90 per cent are diagnosed at an early stage.”
In developed nations, such as the United States, Canada, and across Western Europe, early detection through widespread PSA testing has kept mortality rates significantly lower despite high incidence. India’s mortality rates remain disproportionately elevated, not because the cancer is more aggressive here, but because it is found too late.
Age, Genes, and a Changing Table
There is no single cause of prostate cancer. Instead, a constellation of risk factors, some inherited, some environmental, some simply the consequence of living long enough, collectively raises a man’s likelihood of developing the disease.
Age is the most consistent predictor. As men grow older, their cells divide millions of times, and with each division, there is a small chance of genetic error. Hormonal changes that accompany ageing also play a role. Besides, the immune system weakens over time, a process known as immunosenescence, impairing the body’s ability to detect and destroy abnormal cells before they proliferate. Dr Yawar confirms this: “Patients with an age above 60 years are usually diagnosed with prostate cancer. Rarely do younger patients present with the disease.”
But age and genetics account for only a part of the picture. Lifestyle and environment, experts increasingly argue, are carrying far more of the burden than was once appreciated.
Dr Khalid Zaffar Masoodi, an associate professor and senior scientist in the Division of Plant Bio-Technology at SKUAST Kashmir, frames it plainly: “Out of one hundred per cent of cancer cases, 20 per cent are genetic, and 80 per cent are due to environment, lifestyle patterns, and food habits.”
The shift in Kashmiri dietary culture over recent decades has been rapid and far-reaching. Where earlier generations ate simple, traditionally prepared foods, contemporary diets increasingly feature processed foods, deep-fried snacks, and carbonated drinks.
Dr Masoodi points to a detail that startles many: through the regular consumption of processed and preserved foods, a person today ingests an estimated 60 to 68 kilograms of preservatives annually. He also highlights the issue of plastic water bottles, which contain phthalates, endocrine-disrupting chemicals linked to hormonal cancers.
“People in Kashmir during old times consumed simple and traditional foods which did not cause any harm,” he said. “Rather than continuing with them, we switched to modern and deep-fried foods, which can sound tasty but are disastrous for a human being.”
Cost of Waiting
The symptoms that eventually bring most men to a clinic, weak or difficult urination, pelvic pain, blood in the urine or semen, bone pain, and unexplained weight loss, are not, in themselves, early warning signs. They are indicators of a cancer that has already had time to establish itself and, in many cases, to progress.
“On average, we receive 15 to 20 cases per month,” said the urologist at SKIMS. “These numbers were far lower six or seven years ago.”
The trajectory is clear. A disease that once ranked relatively low among cancers in India now sits in the top three for men. In Kashmir specifically, the combination of low awareness, no structured screening, and a cultural reluctance among men to seek medical help, particularly for conditions related to the urinary or reproductive system, has created the conditions for prostate cancer to advance unnoticed through the population.
Treatment, when cancer is caught early, is highly effective. Active surveillance, involving regular PSA tests, prostate examinations, and periodic biopsies, is the most commonly employed approach for slow-growing, localised disease. Surgery, radiation therapy, hormone therapy, chemotherapy, and androgen deprivation therapy are all available at facilities such as SKIMS.
“Treatment depends on many factors: age, grade, stage, and aggressiveness of disease,” said Dr Yawar. “Some of the common treatments given are active surveillance, surgery, radiation, chemotherapy, androgen deprivation therapy, and palliative care.”
But the effectiveness of every one of these treatments diminishes sharply with each stage of advancement. The fourth stage, at which half of India’s prostate cancer patients are first diagnosed, offers the fewest options and the lowest chances of survival.
A Local Answer
In the midst of this sobering picture, a quiet innovation has emerged from SKUAST Kashmir’s laboratories. Dr Khalid Zaffar Masoodi and his research team have spent the past decade developing what they call Magic Food, a plant-based functional food designed to help prevent or manage prostate-related disease.
The project began in 2015 under the banner of drug discovery from medicinal plants. Over years of laboratory research, the team screened approximately 400 medicinal herbs and crops native to the Kashmir region, identifying compounds capable of inhibiting the growth of prostate cancer cells. From this process, 16 potential anti-cancer molecules were discovered, five of which were derived from edible plant sources already embedded in traditional Kashmiri diets.
“We used these under-utilised foods, which have very high concentrations of beneficial molecules that support a person’s overall health,” said Dr Masoodi. The response, he said, has been considerable. “Almost 70 per cent of the patients who used this food showed signs of recovery.”
The project represents something beyond its immediate clinical promise. It serves as a reminder that Kashmir’s natural and culinary heritage may hold answers. These answers could address problems that modern, processed food culture has helped create.

A Quiet Emergency
Prostate cancer does not announce itself. It does not arrive with immediate pain or visible signs. It grows slowly, silently, and by the time most men in Kashmir learn they have it, the window for the most effective treatment has often passed.
The disease is rising. The awareness is not keeping pace. And the gap between early diagnosis, where survival is high, and late diagnosis, where it is not, is being filled, every month, by 15 to 20 new cases arriving at SKIMS alone.
Fayaz survived. He is grateful and frank about what his experience taught him. The question that now hangs over Kashmir’s public health conversation is how many men, at this moment, are living with the same disease he had, and, like the man he once was, feeling absolutely nothing.