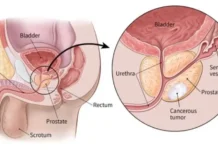
Kashmir, with its rich culinary identity and large consumer market, is grappling with a growing gastric health crisis. Syed Shadab Ali Gillani spoke with gastroenterologist Dr Reyaz Ahmad Para, and Afreen Ashraf brings the highlights of their conversation in black and white
KASHMIR LIFE (KL): Kashmiris complain about “mead doud”. As a gastroenterologist, how do you see it?
DR REYAZ AHMED PARA (RAP): Meadeh doud, as it is commonly called, is not a single disease. The pain can originate from different parts of the digestive system. It may involve the oesophagus, leading to reflux or acidity, or the lower tract, causing conditions such as ulcers or duodenitis. In some cases, gallbladder stones produce pain that is felt near the stomach. Various infections can also disrupt the stomach’s normal functioning. Notably, cardiac conditions are sometimes mistaken for stomach pain, underscoring that what appears to be a routine stomach-ache may have a far more serious cause.
KL: What exactly is acidity, and how does it occur?
RAP: The stomach produces acids that must remain within a specific pH range to maintain a healthy internal environment. These acids kill bacteria, aid digestion by activating enzymes, and help sterilise the food we consume. The key, however, is balance.
When this balance is disturbed, the stomach’s protective mechanisms weaken, leading to acidity. The problem is not confined to the stomach alone. Other parts of the digestive system, particularly the food pipe, lack such strong protection. Repeated acid reflux can therefore cause inflammation of the oesophagus.
If this process continues over a prolonged period, it can alter the lining of the food pipe, potentially leading to serious complications, including malignancies.
KL: Can you tell us how exactly our stomach’s defence mechanism is weakened?
RAP: One of the main factors is a bacterial infection caused by Helicobacter pylori. This bacterium usually enters the body through food or water and is unique because it can survive the stomach’s acid. It changes the stomach’s pH, eventually leading to damage to the lining and leading to more acidity. And if not looked after, it can also contribute to other digestive problems like gastritis, erosions, ulcers, and in serious cases, even gastric cancer.
Other factors that weaken the stomach’s defence include smoking and certain dietary habits. Foods high in salt or containing nitroso compounds, commonly found in preserved, stored, or fermented items, can disturb stomach pH. Stress is another major contributor, as it triggers chemical responses that increase acidity. In addition, underlying conditions such as diabetes or a weakened immune system can impair gastric defences, while long-term use of medications such as steroids and painkillers may further disrupt acid balance.
KL: What will you advise people complaining of acidity?
RAP: From experience, anyone with persistent acidity should undergo proper medical evaluation. The severity of cases seen in Kashmir is worrying, with a notably high number of malignancies. An endoscopy is therefore advisable to rule out serious conditions.
Equally concerning is the practice of self-medication. Many people begin long-term use of drugs such as pantoprazole without medical advice and seek help only when symptoms worsen. This is unsafe. Early consultation and timely evaluation are essential to prevent complications.

KL: Acidity apart, what are the other gastric problems in Kashmir?
RAP: Reflux disease, often linked to obesity and dietary habits such as late-night meals, is common. Another condition frequently seen is hiatus hernia, in which a part of the stomach moves up through the diaphragm, disrupting the valve mechanism and aggravating reflux. Patients may also complain of a dry or blocked throat.
Indigestion and gastro-paresis are more commonly observed in older adults, people with diabetes, and those on long-term medication.
KL: Is vomiting linked to stomach issues?
RAP: Yes, it can happen due to issues in the stomach and also due to issues in the duodenum or small intestine. These issues cause the brain to start a mechanism of vomiting out the undigested food, and sometimes vomiting could be caused by problems in the brain. Besides, vomiting is a side effect of certain medications as well. If vomiting happens occasionally, self-medication may help, but frequent vomiting is a warning sign and should be examined by a doctor.
KL: What causes bloating?
RAP: Bloating is a common complaint. It usually feels like tightness in the abdomen or excessive gas formation, and it involves both the stomach and intestines.
Gas formation is part of digestion, with most gas being harmless carbon dioxide that is expelled through the lungs. Problems arise when gases such as methane and sulphur are produced in excess, leading to discomfort and foul-smelling stools. This often results from undigested fibre, food intolerance, or an overgrowth of harmful gut bacteria.
Bloating may also signal intestinal disease. Cases of inflammatory bowel disease, once relatively uncommon, are now being seen more frequently. In IBD, ulcers, inflammation, and bleeding in the intestines can cause bloating and post-meal pain, and over time may lead to intestinal narrowing and impaired digestion.
Irritable bowel syndrome is a functional disorder in which disrupted brain-gut communication affects normal bowel function. Bloating should not be ignored, as it is often a sign of an underlying gastrointestinal condition.
KL: And constipation is common.
RAP: Constipation is directly linked to gastrointestinal health and is one of the most common reasons people consult a doctor. It can be quite troublesome, as it affects daily life and, in chronic cases, can even impact a person’s mental health.
Constipation is itself a symptom and can reflect a range of underlying conditions. Acute constipation, in particular, warrants medical evaluation and treatment. Perception of constipation also varies widely. Some individuals feel constipated if bowel evacuation feels incomplete, while others are comfortable even without a bowel movement for two or three days.
Medically, bowel habits differ from person to person. Passing stool three times a day or once every three days can both be normal, provided there is a sense of complete evacuation and no warning signs such as bleeding, abdominal pain, or weight loss. Even so, assessment by a doctor is advisable, rather than relying on self-medication.
KL: Is constipation also linked to stress?
RAP: The gut has a complex neural network that is closely connected to our mental health. When a person is under stress or facing mental strain, this network gets affected, which can lead to gut problems.
KL: Are gastrointestinal problems linked to headaches?
RAP: Theoretically, there is no direct mechanism, but I have heard from my seniors and colleagues about patients reporting headaches due to gastric issues. Stress could be a contributing factor, as the gut and brain are connected through a complex neural network.
KL: Intestinal cancers are a growing concern. What should people know about it?
RAP: Lower gastrointestinal problems are common and often present with pain, bloating, bleeding, constipation, or loose motions. Given the relatively high incidence of lower GI cancers here, such symptoms warrant prompt evaluation. While less common than upper GI malignancies, colorectal cancer is still frequently encountered.
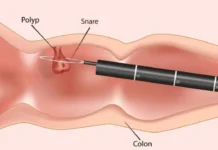
The encouraging aspect is that colorectal cancer is among the most preventable cancers and is well understood in terms of its development. With age- and family history–based screening, small polyps can be detected early and removed during colonoscopy, thereby preventing cancer.
Colorectal screening, therefore, deserves greater attention. Ideally, everyone above 40 years should undergo at least one colonoscopy, even in the absence of symptoms or family history. Accordingly, any patient presenting with lower GI symptoms is advised to undergo colonoscopic evaluation.
KL: What are the symptoms that should lead a person to undergo a colonoscopy?
RAP: For individuals with no symptoms and no family history, colonoscopy is generally recommended between 45 and 50 years of age. Familial colorectal cancers, however, are distinct and include several inherited syndromes. One such condition is familial adenomatous polyposis, in which the colon develops hundreds or even thousands of polyps that can progress to cancer. In these cases, screening must begin much earlier, sometimes from childhood, due to the high inherited risk.
If a person has a first-degree relative with colorectal cancer, screening is usually advised 10 years earlier than the standard age, or earlier based on medical guidance. While it typically takes 10 to 15 years for a polyp to become cancerous, this progression is significantly faster in syndromic families, where screening may be recommended as early as 10 years of age.
KL: Is it inevitable for a person with a family history to develop cancer?
RAP: No, a family history does not make cancer inevitable. It increases genetic risk, which is precisely why screening is critical. Colonoscopy is a straightforward test that allows direct visualisation of the intestines, and early detection and removal of polyps can prevent progression to cancer.
In many countries, routine screening for gastrointestinal malignancies is part of national health programmes and is covered by insurance. Such organised screening is still lacking here, and these tests are not state-funded. Timely screening, however, remains one of the most effective ways to prevent cancer.
KL: Why are gastrointestinal cancers rising in Kashmir?
RAP: Based on clinical experience, observational data, and studies by reputed institutions, upper gastrointestinal cancers are notably more common in Kashmir. Some studies indicate that gastric cancer rates here are six to ten times higher than in many other regions.
This makes it imperative that gastric symptoms are never ignored. Of particular concern is the increasing number of very young patients, sometimes aged between 27 and 35, being diagnosed with upper GI cancers, cases that were rarely seen during years of practice outside Kashmir.
The causes are likely multifactorial, with genetic susceptibility and environmental influences, especially dietary habits, playing significant roles. Internationally, countries such as Japan have faced similar burdens but have successfully reduced mortality through strict screening programmes. A comparable emphasis on early and systematic screening is urgently needed here.
Many cases are still detected at advanced stages, often stage three, when treatment options are limited. Early-stage cancers, by contrast, are frequently treatable or curable, underscoring the critical importance of screening and early diagnosis.
KL: Is nun chai (pink salt tea) one of the reasons behind gastrointestinal problems in Kashmir?
RAP: Nun chai has been under discussion for some time, with some studies linking it to upper gastrointestinal diseases, including malignancy. The risk, however, lies largely in the manner of consumption. Nun chai contains high amounts of salt and soda, and when consumed piping hot, it can irritate the stomach lining and mucosa.
Taken in mild to moderate quantities, it does not pose a significant risk, and people can continue to enjoy this traditional beverage.
Logically, consuming any hot beverage on an empty stomach can irritate the gastric lining. Since nun chai contains salt and soda, this effect can be more pronounced. It is therefore advisable to consume it after eating and to prepare it with reduced salt and soda to minimise its impact on gastric health.

KL: Other than nun chai, what dietary habits in Kashmir affect gastric health?
RAP: In Kashmir, preserved foods like hokhsuen (dried vegetables) are widely consumed, reflecting a long-standing tradition. The concern arises when preservation methods are unhygienic, allowing fungal growth that produces harmful nitroso compounds, which can irritate the stomach lining.
Local food preservation departments can play a key role in educating people about safer, scientific methods. Pickles, another common dietary item, are high in salt and can affect gastric health, but when consumed in moderation, they can still be enjoyed safely.
KL: Is wazwan problematic for gastric health?
RAP: Wazwan can be enjoyed in moderation, provided it is prepared using healthy practices, avoiding additives and processed ingredients, and using natural spices. Ultimately, moderation is the key to maintaining good gastric health.
KL: Patients with stomach pain are advised to avoid tomatoes and sour foods.
RAP: Sour foods, like citrus fruits, can stimulate stomach acid, but they need not be completely avoided. It is best not to consume them on an empty stomach, especially for those experiencing acidity or ulcers.
KL: And curd?
RAP: Curd is healthy when pure and hygienically prepared. Rich in probiotics, good fats, and essential minerals, it supports digestive health and is beneficial for the stomach when consumed properly.
KL: Rice is our staple meal. What do you say?
RAP: Rice, a staple for Kashmiris, is a good source of carbohydrates and essential energy. Rising issues like obesity, fatty liver, and diabetes have led some to cut back on rice, but the real culprit is a sedentary lifestyle. With regular physical activity, rice can be included in the diet safely, as unused energy, not the rice itself, contributes to fat accumulation.
KL: Fatty liver is now common.
RAP: Fatty liver is not just a concern in Kashmir; it is a growing global problem. Over the past 30 to 40 years, fatty liver disease has become one of the most common liver conditions, surpassing many others, such as hepatitis.
The disease occurs when fat in the liver exceeds normal levels, normally around 5 per cent. Excess fat causes liver cells to enlarge and the organ itself to grow. Over time, these cells can produce harmful substances that damage the liver. Initially, fat accumulation is reversible, but if it progresses to steatohepatitis, the condition becomes more serious yet still manageable. Without intervention, it can advance to fibrosis, shrinkage of the liver, cirrhosis, and eventually liver failure or cancer.
The condition is now termed metabolic-associated steatotic liver disease (MASLD), previously called non-alcoholic fatty liver disease, due to its similarity to liver damage from alcohol. The main cause is weight gain from an imbalance between energy intake and expenditure. Unburned energy accumulates as fat in the liver, while insulin resistance further contributes to fatty liver, obesity, diabetes, and other metabolic disorders.