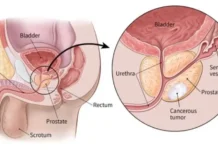
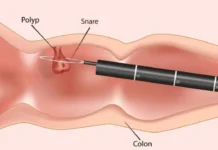
Breast cancer is steadily emerging as the leading cause of cancer-related deaths among women in Kashmir. In a detailed conversation with Kashmir Life, noted breast cancer surgeon Dr Shabnam Bashir discussed the scale and challenges of the crisis, condensed by Afreen Ashraf for clarity and readability
KASHMIR LIFE (KL): What is the state and status of breast cancer in Jammu and Kashmir?
DR SHABAM BASHIR (SB): Globally, breast cancer affects an estimated 2.3 million women each year. In India alone, nearly 2.5 lakh women are diagnosed annually. However, data from the European Cancer Registries suggest that these figures capture barely one-third of the actual burden, as they rely primarily on hospital-reported cases, underscoring the true magnitude of the problem.
The situation becomes even more alarming when viewed at the regional level. Breast cancer remains the leading cause of cancer-related mortality among women, particularly those in the reproductive age group. Disturbingly, nearly 60 per cent of patients are diagnosed at Stage III, an advanced stage where outcomes are often poor. Recent estimates indicate that for every two women diagnosed, only one receives timely treatment, largely due to delays in detection.
This is especially tragic given that early-stage breast cancer is highly curable, with survival rates ranging from 90 to nearly 100 per cent when diagnosed and treated in time.
KL: Is there any reliable data indicating how many women are diagnosed with breast cancer each year in Kashmir?
SB: Data released by state and regional cancer registries, including those from SMHS and SKIMS, reveal that nearly 38 new cancer cases are diagnosed daily. Of them, three to five instances involve women diagnosed with breast cancer.
KL: Based on your professional experience, how has the pattern of breast cancer changed over time, and what key factors contribute to its onset?
SB: Cancer is a multi-factorial disease. We are continually exposed to carcinogenic factors that increase cancer risk, though their impact varies based on genetic susceptibility and the intensity and duration of exposure. Breast cancer risk factors are broadly classified as modifiable and non-modifiable; addressing the modifiable ones alone could potentially prevent 30-50 per cent of cases. While breast cancer predominantly affects women, men can also develop the disease, albeit rarely.
Beyond genetic and non-modifiable factors such as ethnicity, height, and breast density, several lifestyle-related risks play a critical role. Smoking is a major preventable trigger. Smoking-related breast cancers also tend to be biologically more aggressive.
Obesity is another significant risk factor, as excess body fat is converted into estradiol, a hormone that fuels breast cancer growth. Even women of normal weight face increased risk if they lead physically inactive or sedentary lives; in fact, inactivity itself is an independent risk factor.
Reproductive factors further influence risk. Late first pregnancy, particularly between 30 and 40 years, and delayed or reduced breastfeeding increase vulnerability. The growing use of hormone replacement therapy for reproductive and menopausal issues has also contributed to the rising risk.
Besides, exposure to carcinogens such as certain plastics, cosmetics, and radiation therapy can elevate breast cancer risk. Hormonal medications prescribed in cases of recurrent abortions may also increase future breast cancer risk, including potential effects on female offspring.

KL: With evolving societal trends, such as sedentary lifestyles, delayed marriages, rising rates of PCOD, and infertility, do these factors collectively contribute to the increasing burden of breast cancer?
SB: Breast cancer has increasingly emerged as a disease shaped by lifestyle and urbanisation. The lifetime risk is significantly higher in urban areas than in rural settings, about one in 22 women in cities compared to one in 60 in rural regions. PCOD is another growing concern; among every two to three women diagnosed with breast cancer, one is found to have PCOD.
When viewed within the broader cancer burden, nearly 30 per cent of cancers are linked to smoking, 30-35 per cent to unhealthy lifestyles and poor diet, and another 25-30 per cent to infections. What is striking is that a large proportion of these risk factors are preventable.
Unlike Western countries, where breast cancer typically occurs after the age of 50, Kashmiri women begin facing risk around 40, with the disease appearing nearly a decade earlier. Genetic factors also play a role. The prevalence of consanguineous marriages has amplified inherited risks, particularly mutations in the BRCA1 and BRCA2 genes, contributing to an alarming rise in breast cancer cases among women under 30.
Societal norms have undeniably shifted. Late marriages and delayed childbirth are established risk factors, but they cannot be viewed in isolation. Breast cancer is also seen among women who marry early, conceive young, and breastfeed, underscoring that no single factor is solely responsible.
While no single cause can be identified, addressing modifiable risk factors is essential to reducing the overall cancer burden. Breast cancer is fast becoming a public health emergency, a looming crisis that demands immediate and sustained preventive action.
KL: What steps can women take to reduce their risk, and which early warning signs are crucial for the timely detection of breast cancer?
SB: Kashmir remains a conservative society where open discussions about breast health are often difficult. The first and most critical step is to break this taboo. Awareness must be driven through print and digital media, videos, seminars, and community programmes, and these efforts should not be limited to women alone. Men must be actively involved. The core message should be simple and clear: it is acceptable to talk about one’s body when it concerns health. Only then can meaningful progress be made.
Breast health awareness should begin early. While breast self-examination alone may not significantly reduce mortality, many women are unfamiliar with their own bodies and therefore struggle to recognise abnormal changes. Awareness, in this sense, is about familiarity, knowing what is normal in order to detect what is not.
Medical bodies such as the Association of Breast Surgeons of India are working to spread awareness, but education must reach the grassroots. Mothers should educate their daughters from puberty onwards, encouraging comfort and confidence in noticing unusual lumps or changes. This familiarity significantly enhances the likelihood of early detection.
Breast health education should also be incorporated into school curricula and taught in a scientific, open, and non-alarming manner. Early, informed education can reduce fear, prevent late diagnosis, and ultimately save lives.
Men, as central figures in family structures, also have a responsibility to support the health of their wives, daughters, and mothers. Women, in turn, should avail themselves of appropriate diagnostic measures for early detection and consult qualified healthcare professionals rather than relying on informal advice, which can delay treatment and worsen outcomes.

KL: Do we currently have adequate infrastructure to manage this growing crisis?
SB: We do have infrastructure in place, but the real question is how effective and sufficient it is. At present, only a handful of well-equipped centres are available to manage the burden of cancer care. State and regional cancer centres are overwhelmed with patients, often leading them to remain on the waiting list for weeks, which delays treatment.
Private hospitals, such as Paras Hospital, are also witnessing a heavy patient footfall. Overall, we do possess basic facilities that are helping us manage the situation. However, the existing bed capacity is inadequate and needs expansion. In Kashmir, chemotherapies, immunotherapy, or precision oncology therapy services are available. Kashmir also has two radiation therapy centres. We also have surgical oncologists in both private and government sectors.
However, there is also a need for modern equipment, dedicated cancer centres, and tailor-made oncology facilities that can provide care for evolving cancer.
Our hospital has introduced advanced, modern cancer treatment technologies in Kashmir. Our goal is to ensure patients receive high-quality care locally, without needing to seek treatment outside the region. This requires strengthening and reinforcing existing healthcare facilities. This can only be achieved through coordinated efforts between the government and the private sector. Each year, Kashmiris spend nearly Rs 13-14 crore on treatment outside the region due to limited trust in local healthcare. Building confidence and strengthening medical infrastructure within Kashmir is, therefore, essential.
KL: In breast cancer, is surgery inevitable?
SB: When cancer is detected early, surgery remains the primary treatment. Advanced-stage cancers are best managed with chemotherapy, provided it is administered accurately and appropriately. Before initiating treatment, each case is reviewed by a multidisciplinary tumour board to determine the optimal approach. To date, there is no evidence warranting a change in these established treatment protocols, even in advanced disease.
KL: Cancer-related surgical procedures are expensive. How can these costs be managed?
SB: Health must be our foremost priority. As a society, we often spend generously on weddings, clothing, and personal care, yet hesitate when it comes to healthcare. Government and private hospitals operate under different models; the private sector, focused on timely and effective treatment, must invest in quality standards, infrastructure, and services, which inevitably raise costs. We must recognise this reality, rethink our financial priorities, and approach healthcare as a shared social responsibility.
KL: Can breast cancer be managed within the limitations of the Golden Card in Jammu and Kashmir?
SB: At present, health insurance schemes struggle to meet the actual costs of care in private hospitals. While designing insurance policies, governments and policymakers must consult healthcare providers to realistically account for the cost of infrastructure, equipment, and advanced medical technologies. Such alignment is essential to ensure sustainable, high-quality treatment. At the same time, society must reassess its spending habits and place a greater priority on investing in health.
KL: What are the problems a patient can face after they undergo surgery?
SB: Cancer patients face multiple challenges that must be addressed comprehensively. These include lymphedema, onco-nutrition needs to improve tolerance to surgery and therapy, and pain management, especially in advanced stages, under the care of pain specialists. Psycho-oncological support is also essential to help patients manage the psychological impact of the disease.
Breast cancer patients require long-term follow-up, often extending up to 20 years. During the first five years, when the risk of recurrence is highest, patients are reviewed every three months. Thereafter, follow-up intervals are gradually extended once the patient is confirmed to be disease-free.