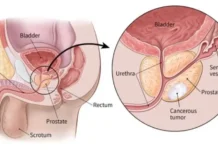
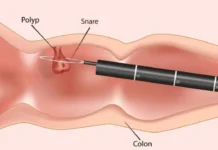
In Kashmir, life for those with rare blood disorders unfolds quietly, beneath the surface of public health narratives. Marked by genetic legacies, strained healthcare systems, and daily battles for survival, their stories are often written in invisible ink felt but rarely seen, Babra Wani reports
His skin shifts colours, turning pale, red and sometimes blue. In a modest home in Kulgam, Zafar, 12, spends most of his days indoors, distanced from the carefree childhood of his peers. He appears frail, his face drawn from years of enduring a rare bleeding disorder. Even a small bump or an emotional outburst can set off prolonged bleeding, at times from his nose or mouth. For his father, this has been a relentless ordeal since 2018, when Zafar’s condition was first diagnosed.
“He was just five years old,” his father recalled, his voice low with fatigue. “He would bleed suddenly, even in his sleep. There were days we woke up to find his pillow soaked in blood. At first, the local doctors could not understand what was wrong.”
Zafar’s father, Ghulam Ahmad, 45, used to sell goods from a cart to make ends meet. He says he lacked the money and awareness to find a proper diagnosis. For two years, he moved from one hospital to another, exhausting his savings, but no doctor could offer clarity.
After repeated tests and referrals, the doctors eventually diagnosed Zafar with a rare clotting disorder similar to haemophilia, requiring regular infusions of Factor VII, a clotting agent. Ghulam said the treatment does not always work. Sometimes it helps, sometimes it does not. Zafar continues to bleed. Even brief play or distress can trigger a nosebleed. He cannot attend school regularly. The third grader attends school when health permits.
Ghulam remembers the desperate trips in search of a cure. He was advised to take Zafar to Delhi. He sold a piece of land and travelled there. Doctors informed him that extensive tests and treatment would cost nearly one lakh rupees. He went through with the tests. Later, another doctor recommended bone marrow therapy, which would cost Rs 25 lakh. Shocked over the costs, he broke down in front of him. Another doctor took him aside and advised against it. He was told not to waste his money. It was a genetic condition with no permanent cure.
Those words destroyed what little hope he had left.
The Diagnosis
Zafar was eventually diagnosed with Glanzmann thrombasthenia, or GT, a rare inherited bleeding disorder. It typically appears as mucocutaneous bleeding and severe haemorrhage following injury or surgery. Although patients have a normal platelet count, their platelet function is impaired, leading to prolonged bleeding time.

Doctors assert bleeding is generally managed through platelet transfusions, while bone marrow transplantation has been attempted in a few rare cases. With proper supportive care, the overall prognosis of GT is considered positive.
According to Syed Majid Qadri, who works closely with patients suffering from rare blood disorders in Kashmir, the situation is more severe than commonly perceived.
“In Kashmir, we have almost eleven registered patients with GT, as it is medically known,” he explains. An extremely rare clotting disorder, children affected by it suffer frequent and uncontrollable nosebleeds. In emergencies, doctors rely on palliative care, primarily using Factor VII injections, which are the only way to temporarily manage bleeding. However, this is not a cure. These families live in constant fear. Even a minor injury or spontaneous episode can become life-threatening.
Endless Vigil
At home, life became a continuous loop of care and anxiety. Zafar’s father had to stop working consistently after developing serious health issues of his own, including a benign brain tumour, likely worsened by years of unrelenting stress. “I was a street vendor, selling clothes on a cart,” he said. “I left in the morning and came back in the evening. But after Zafar fell sick, my life turned upside down. Now I cannot even do heavy work because of my tumour. The doctors say surgery is risky. I just take medicines and go for an MRI every six months to see if it is growing.”
Managing Zafar’s illness on an unstable and insufficient income became overwhelming. “To travel from Kulgam to Srinagar for treatment costs Rs 1,000 each time. Sometimes I have to stay overnight. There were days I slept outside the blood bank in Srinagar, waiting for platelets. Once I went at midnight, but they told me to wait until 10 am. I sat there crying, holding my son, feeling helpless.”
The emotional burden, however, cut even deeper. Zafar had come to understand more than any child should. “He sometimes says he does not want to live like this. He asks me, ‘Why can’t I play like other children? Why can’t I run with my sisters? Why does my face turn blue when I go to school?” His father pauses, holding back tears. “How do you answer a child when he says things like that? I tell him he will be fine, but inside, I know the doctors have said there is no cure.”
Despite the bleak medical outlook, the family tried to preserve a sense of normalcy. Zafar’s two younger sisters, aged eight and three, went to school and played outside. “They do not have the disorder,” the father said. “They live a normal childhood. But Zafar watches them from the window. He wants to join them, but if he plays for too long, he bleeds, and his face turns pale by evening.”

The illness also led to a quiet social isolation. “When you are in trouble, people slowly stop coming. At first, everyone felt sorry. But as time passed, they stopped visiting. They have their own lives. You realise in the end that you have to walk this path alone,” he said.
What sustained him was his unwavering love for his son. “Everyone in the village says that if it were anyone else, they would have given up. But I can’t. I ask God to keep me alive as long as Zafar is here, because no one else can look after him the way I do.”
Doctors had made it clear that Zafar would live with the condition for as long as he lived. “There is no hope for a complete recovery. Even in Delhi, the best doctors said the same thing. They told me to take him home and just give him care. No amount of money or tests will change his condition.”
Yet Ghulam still clung to prayers, however small, and to moments of love. “I just want him to have less pain. I want him to smile, to go to school without fear, to play a little without bleeding. I do not dream of miracles anymore; I only dream that his suffering becomes less.”
He remembered the humiliation he endured at the hands of doctors at SKIMS, who treated him with indifference due to his repeated visits. “Once, a doctor said that your son is not going to make it. He addressed his colleagues and said, iss dangar ko maene kaha bhi bohat baar (I have told this idiot many times). It was so humiliating, but I endured everything for my son.”
Beyond Zafar
GT apart, Majid Qadri pointed out that Kashmir also has a significant number of thalassaemia cases. “At Government Medical College, there are about thirty-five registered thalassaemia patients, while the Children’s Hospital has fifty-five more. These children require regular blood transfusions, sometimes every month, sometimes every 15 days, because their red blood cells break down faster than normal. But the transfusions come with their complications. Dead blood cells can enlarge the spleen, causing pain and further health risks. And repeated transfusions lead to iron overload, which damages organs.”
The risks posed by iron overload were particularly severe. “It can cause heart problems, kidney failure, and severely impact growth. Their facial features may never develop normally. Their height and body shape often remain different from healthy children. To manage this, they need daily iron-chelating medicines to remove excess iron from the body. But here is the tragedy: patients in Jammu are at least getting these medicines through welfare support. In Kashmir, many patients at GMC Srinagar do not even receive those basic medicines. Families have to either buy them at a high cost or simply go without.”

Although some thalassaemia patients could be cured through a bone marrow transplant, the procedure was not feasible for all. “Bone marrow transplant works only if there is a perfect donor match. And it is usually successful only in children; adult patients cannot benefit from it. Even for eligible children, the costs and complexities are beyond the reach of most families here.”
For Qadri, the greatest hurdle was the absence of infrastructure and awareness. “These are lifelong conditions. They do not just affect the child; they change the entire family’s life. Without proper support, without access to medicines and specialised care, families are left feeling helpless.”
Zubair is one of around 100 patients in Kashmir suffering from thalassaemia.
Borrowed Blood
When Zubair was just six months old, his parents began noticing signs of something deeply troubling. He appeared unusually pale and weak, with frequent high fevers that left him drowsy and gasping for breath. After weeks of anxious visits to local doctors in Baramulla, they were referred to PGI Chandigarh, where the diagnosis shattered their world: Zubair had thalassaemia major, a rare genetic blood disorder that prevents the body from producing healthy red blood cells.
Now 24, Zubair speaks with a calmness shaped by years of struggle. “I do not remember life before this,” he said. “Thalassaemia has been with me for as long as I can remember. It is a part of who I am.”
His family, originally from Baramulla, migrated to Srinagar, where they now live and work. Zubair completed his degree in Electronics and Communication Engineering. Despite living with a chronic illness, he remained focused on his aspirations. “I do not want to live differently from anyone else. I studied like everyone, played like everyone, and I want to build a future like everyone.”
Routine of Survival
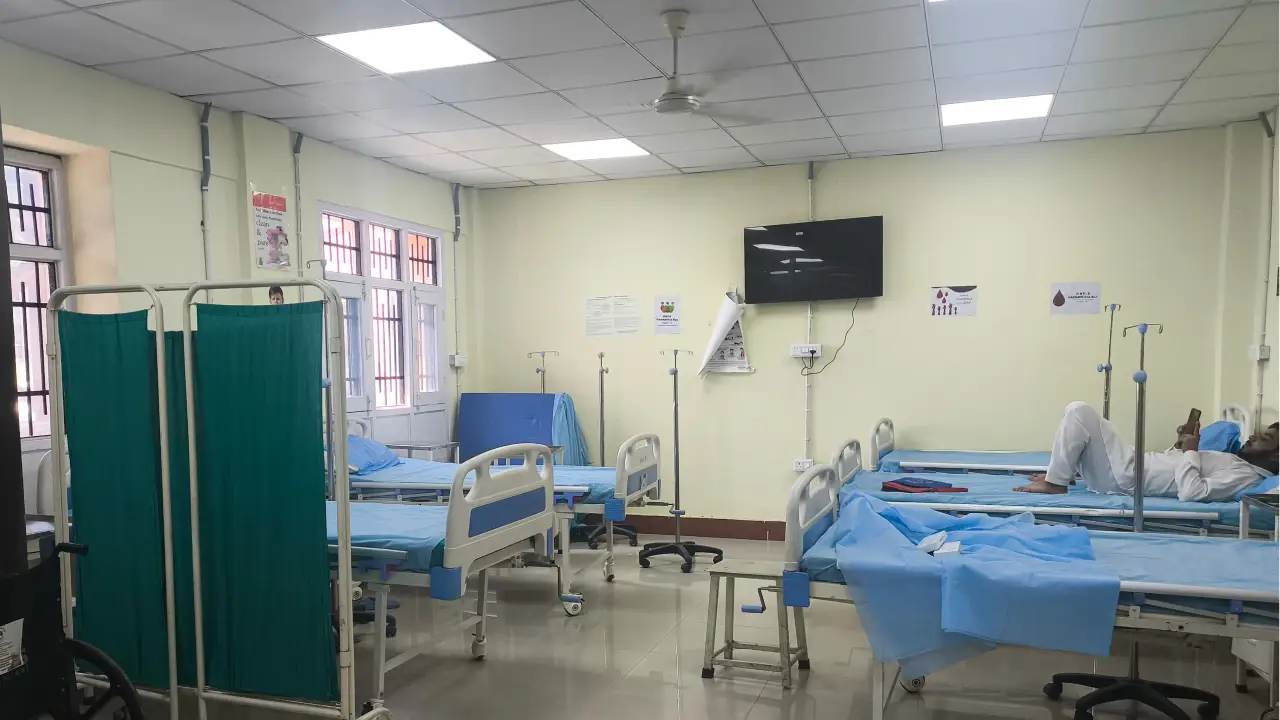
Every 15 days, Zubair undergoes a blood transfusion, a process essential to keeping him alive. “It is not painful, but it is tiring, mentally more than physically,” he said. The transfusion itself, however, is only one part of a larger ordeal. “The real problem is not the transfusion. It is the lack of proper care. We do not have a dedicated thalassaemia ward here. We are put in rooms with patients who have tuberculosis, kidney issues, or other serious infections. For someone who already has a fragile condition, that is dangerous. You are constantly worried about catching something else.”
In search of better care, Zubair often travels to Jammu, where Dr Sanjeev oversees registered thalassaemia patients. “In Srinagar, there is no permanent solution. There is a day care ward in the super-speciality hospital, but it is not well-equipped for thalassaemia. Every few months, we have to go to Jammu. It is an extra burden, not just financially, but emotionally.”
The Cost of Staying Alive
The illness imposes a heavy financial strain. Repeated transfusions result in iron overload, which can damage internal organs if not treated. Zubair explained that this must be managed with iron-chelating medicines. “Medicines like Deferasirox or Deferiprone are crucial; otherwise, the excess iron damages your organs. If I were to buy them from the market, it would cost around Rs 5,000 a month. Luckily, the National Thalassaemia Society in Jammu provides them, but even then, we still have to manage regular check-ups and travel.”
He described the absence of local welfare support as another silent burden. “In Kashmir, we do not have a proper welfare society for thalassaemia. There are only two societies, one in Delhi and one in Jammu. Here, we have about 35 registered patients in GMC Srinagar, but we know there must be more people out there, undiagnosed or silently struggling without treatment. Awareness is very low.”
Pushing Through Limits
Zubair insists that his life is more than his illness. He credited his parents for never holding him back. “They never told me to sit back or avoid playing. They wanted me to feel normal. I went to school, made friends, and did everything my peers did. Even now, I do not let it stop me. I have completed my BTech, and I am preparing for the GATE exam to do my MTech. I want to move ahead, like anyone else.”
Still, the physical consequences of thalassaemia remain present. “The transfusions increase iron in the body, which can cause bone pain, stunted growth, or organ problems. Some people face complications like dislocated joints or hormonal issues. I have been lucky so far, but I know the risks. It is a lifelong thing; you just manage it.”
When asked about his future, including marriage and family, he replied without hesitation. “Doctors say it will not affect my marital life or having children, so I am hopeful. Thalassaemia does not stop you from dreaming. It just makes you more aware of life, more grateful for what you have.”
Zubair’s voice grew firm as he spoke of what must change. “We need a dedicated ward for thalassaemia patients in Kashmir, proper doctors here, and timely access to medicines. Right now, we are forced to rely on Jammu. We need local facilities so patients do not have to keep travelling. We need awareness so families can test for thalassaemia traits before marriage and prevent future cases.”
His words, quiet but resolute, echoed the struggle of many others like him: young lives shaped by pain, but anchored in hope.
Beyond the Familiar
According to experts, thalassaemia is a genetic blood disorder caused by the body’s inability to produce sufficient haemoglobin, a key protein found in red blood cells. “Without sufficient haemoglobin, red blood cells cannot function properly, have a shorter lifespan, and fewer healthy cells circulate in the bloodstream.”
Red blood cells are responsible for delivering oxygen, which acts like fuel for the body’s cells. When there are not enough healthy red blood cells, less oxygen reaches tissues and organs, leading to fatigue, weakness, and shortness of breath, a condition known as anaemia. “In thalassaemia, anaemia can range from mild to severe, and in serious cases, it can damage organs and even become life-threatening.”
For Zubair, the fight was never only personal. It became about easing the path for others like him. “We manage, but it should not have to be this hard,” he said. “No one should have to feel that survival is a privilege.”
Apart from haemophilia, thalassaemia, and Glanzmann thrombasthenia, other rare blood conditions have also been documented. These include platelet function disorder and fibrinogen deficiency. Both affect the blood’s clotting process at various stages. Platelet function disorders occur when the platelet count is normal, but their function is impaired. This leads to symptoms such as easy bruising, nosebleeds, heavy menstrual bleeding, and prolonged bleeding after injury or surgery. These conditions may be inherited or acquired due to medication or illness. Treatments include desmopressin or platelet transfusions.
Fibrinogen deficiency results from the absence or malfunction of fibrinogen, a protein vital for stabilising blood clots. The deficiency can cause severe or uncontrollable bleeding, often visible from birth, and may be hereditary or acquired due to illnesses such as liver disease.
Localised Genetic Traits
Various studies have revealed a local pattern in inherited blood disorders. Kashmiri thrombocytopenia and hereditary stomatocytosis are among the most commonly observed inherited giant platelet disorders in the region. Researchers have also noted significant frequencies of certain ABO and Rh blood groups among different populations in Kashmir.
A study titled Inherited Giant Platelet Disorder, Kashmiri Thrombocytopenia, a Common Syndrome Found in Srinagar, India reported a high prevalence of an autosomal dominant form of inherited giant platelet disorder (IGPD), characterised by mild to severe thrombocytopenia among the Muslim population in the Valley. Among 830 healthy male blood donors aged 15 to 55 years, 15 per cent were found to have thrombocytopenia, with significantly lower platelet counts (mean 109.6 compared to 189.9 in controls, p<0.0001) and larger platelet sizes (mean platelet volume 12.53 compared to 9.52 fl). These individuals did not report a history of bleeding or show other systemic conditions.

Family studies conducted across seven Kashmiri families confirmed the autosomal dominant nature of inheritance affecting both genders. Neonatal analysis showed that 18 per cent of newborns had low platelet counts. Genetic screening ruled out known IGPD-related genes, including MYH9, and SNP mapping identified potential regions on chromosomes 5, 9, and 10 for further research. The findings pointed to a distinct congenital thrombocytopenia syndrome, termed Kashmiri thrombocytopenia, and called for continued genetic investigations to identify the causative mutation.
According to a 2015 study titled Hereditary stomatocytosis: First case report from Valley of Kashmir, researchers documented the first case of hereditary stomatocytosis in the region in a 10-year-old boy. At the time, the condition had only been reported in eight families globally. “Stomatocytes are red blood cells with a slit-like or mouth-shaped central pallor on smears and appear bowl-shaped in wet preparations due to their uniconcave shape. They can form in vitro when certain drugs alter the lipid bilayer of the cell membrane. Hereditary stomatocytosis, also called hereditary hydrocytosis or overhydrated stomatocytosis, is a rare autosomal dominant haemolytic anaemia caused by abnormal sodium permeability in red cell membranes,” the study reads.
(Note: Some names in this story have been changed to protect the privacy and identities of individuals, especially those sharing personal medical details.)