A cure to the Covid-19 disease triggered by Coronavirus (SARS-CoV-2) is too distant but there are a lot of things that we must know about the invisible creature that has jammed the world.

Question: Is Coronavirus laboratory manufacture?
Answer: Firm believers in conspiracy theories insist the Coronavirus (SARS-CoV-2) that has jammed the world with nearly 20,000 deaths is from biological warfare arsenal.
A US News & World Report, however, said that the new Coronavirus arose from natural causes and was not concocted in a lab. “SARS-CoV-2, the virus that causes Covid-19 illness, shows zero evidence of being artificially engineered”, reported a team of scientists who published their findings in Nature Medicine. “By comparing the available genome sequence data for known Coronavirus strains, we can firmly determine that SARS-CoV-2 originated through natural processes,” the study co-author Kristian Andersen, an associate professor of immunology and microbiology at Scripps Research, said. Andersen was joined by scientists from Columbia University in New York City, the University of Sydney in Australia, and Tulane University in New Orleans.
The Coronaviruses have existed for a very long time. There are seven common cold-causing Coronavirus known to mankind. Four of these (229E, HKU1, OC43 and NL63) are seasonal and typically cause mild respiratory infection — fever, cough, nasal congestion, and headache. The remaining three (MERS (2012), SARS (2003) and Covid-19) could lead to life-threatening pneumonia. Many people including US president, Donald Trump, and a wide range of scientists think the virus stop spreading in increased temperatures. But the hardcore scientists say it is slightly too early and will be clear within a month.
After Chinese scientists mapped the genome of SARS-CoV-2 and made that data freely available to scientists worldwide, Andersen and colleagues examined the genetic template for proteins on the outside of the virus, called spike proteins. SARS-CoV-2 uses these proteins to latch onto the host cell. Digging deeper, the researchers looked at the evolution of key components of the spike protein.
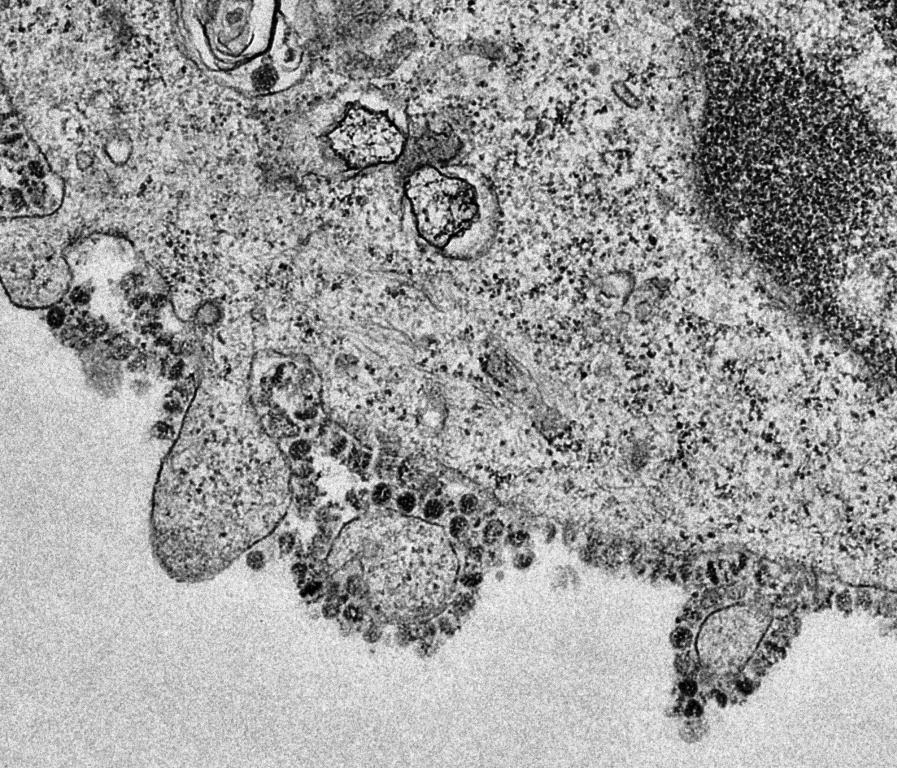
“One component, called the receptor-binding domain (RBD), is a kind of “grappling hook” that SARS-CoV-2 uses to grip human cells. The RBD of the new virus is incredibly effective at binding to the cell – so effective, in fact, that the scientists believe it could only have evolved through natural selection,” the report said. “Another piece of evidence supporting a natural origin for the virus comes from what the researchers called the “backbone” of SARS-CoV-2 — its basic molecular structure. The team reasoned that if scientists were going to synthetically create a new virus in a lab, they’d need to borrow its molecular underpinnings from a virus already known to make people sick. But the molecular backbone of SARS-CoV-2 bears no resemblance to any known Coronavirus that already infects humans. Instead, it closely resembles Coronaviruses found in bats and armadillo-like mammals called pangolins — adding weight to the theory that the new virus made a recent jump in China from animals to people.”
Q: Who is the most potential victim of the virus?
A: Everybody, man, woman and children can be a victim. However, empirical studies in disease-infected belts suggest that the particular virus is spearing women and children in comparison to men. “In Italy, which is the second hardest-hit country behind China, men make up almost 60 per cent of confirmed cases of the virus, and more than 70 per cent of those who have died,” the American website The Hill reported. “Data from China’s Centre for Disease Control showed nearly 64 per cent of deaths in tens of thousands of cases were male, compared to 36 per cent that were female. Meanwhile, in South Korea where 61 per cent of confirmed infections have been in women, 54 per cent of fatalities were made up of men, according to The Washington Post.”
Based on mere empirical studies, Chinese scientists have claimed that people with type A blood are significantly more likely to catch Coronavirus than those with type O. It needs other supporting corroboration. Smokers, older people, especially with diabetes, high blood pressure and other chronic issues are likely to face serious issues, if infected.
Q: What are the basic symptoms of an infection?
A: After looking at 55924 cases, the WHO found 87.9% had a fever or a dry cough (67.7%), or both. Less common symptoms were fatigue (38.1%), coughing up phlegm (33.4%), shortness of breath (18.6%), sore throat (13.9%), headache (13.6%), joint pain (14.8%), chills (11.4%), nausea or vomiting (5%), nasal congestion (4.8%), diarrhoea (3.7%), coughing up of blood (.9%) and eye discharge (0.8%).

“Fever and cough was observed in almost all COVID-19 patients described in the literature,” Jan Carette, associate professor of the Department of Microbiology and Immunology at Stanford University School of Medicine in Palo Alto, told sfgate.com. “Only very few cases had prominent upper-respiratory-tract signs and symptoms (eg, runny nose or sneezing). This means that the virus likely hangs out more in the lower airway rather than the upper airway.”
The WHO analysis also revealed that most people develop symptoms on an average of five to six days after infection, though the range is anywhere from one to 14 days.
However, Fox News quoted a study published in The American Journal of Gastroenterology by Chinese researchers who have found – on basis of data from 204 Coronavirus patients in Hubei province – that early symptoms could come from gastrointestinal issues. Of the 204, 99 (48.5%) reported to the hospital with “with one or more digestive symptoms as their chief complaint,” like diarrhoea, vomiting or abdominal pain.
“Of these 99 patients, 92 developed respiratory symptoms along with digestive symptoms, and 7 presented with only digestive symptoms in the absence of respiratory symptoms. Among the 105 patients without digestive symptoms, 85 presented only with respiratory symptoms, and 20 neither had respiratory nor digestive symptoms as their chief complaint,” Fox News quoted the authors writing.
“Anosmia, the loss of sense of smell, and ageusia, an accompanying diminished sense of taste, have emerged as peculiar telltale signs of Covid-19, the disease caused by the coronavirus, and possible markers of infection,” The New York Times reported. “British ear, nose and throat doctors, citing reports from colleagues around the world, called on adults who lose their senses of smell to isolate themselves for seven days, even if they have no other symptoms, to slow the disease’s spread.”
Q: Can the infection spread in the neighbourhood?
A: Mere presence of an infected patient at home or in the neighbourhood does not necessarily mean, one gets infected unless the precautions are not taken care of, especially social distancing. Infected are supposed to remain in the hospital in isolation. The infection spreads by transfer of virus in close contact by way of coughing, sneezing, shaking hands and hugging.

The virus does not stay longer in the air once released from an infected body. Public health authorities have been asserting that the virus spreads when someone sneezes or coughs, creating “respiratory droplets,” which will quickly land on nearby surfaces or people as opposed to hanging in the air. These droplets can land in the mouths or noses of people who are nearby or possibly be inhaled into the lungs.
A single cough, sfgate.com reported produces up to 3000 ultra-fine droplets that can float around in still air for three hours. The study was carried out by the National Institutes of Health and Princeton University scientists and published in the New England Journal of Medicine. “In turbulent air — for example, a setting in which air is circulated in an unfiltered air-conditioning system — the aerosol droplets tend to settle faster on surfaces,” the study said.
A study carried out by the American National Institute of Health has found that the Coronavirus survives on plastic-made electronics, such as a keyboard or mouse, for up to three days, and cardboard for up to 24 hours. On steel, it can survive for 48 hours. All this experimentation is in laboratory conditions. A general belief is that the virus dies more rapidly in hotter environments and the presence of sunlight.
Q: How fast does the virus spread?
A: A study carried out on nine infected patients at Munich Hospital in Germany said that Coronavirus can spread before it causes symptoms and for as many as 12 days after the recovery. The Covid-19 causing virus triggers more virus shedding in comparison to SARS.
“In SARS, it took 7 to 10 days after onset until peak RNA concentrations (of up to 5×105 copies per swab) were reached,” the researchers wrote. “In the present study, peak concentrations were reached before day 5, and were more than 1,000 times higher.” Seemingly, this makes the novel Coronavirus far harder to contain. SARS was contained after about 8,000 cases. The infected have shown a high viral shedding — meaning people are very contagious — during the first week of symptoms. “This could mean very high transmission of the virus before those infected show any clinical symptoms at all, or when they are only beginning to experience very mild symptoms and are still going about their daily routines, according to Michael Osterholm, director of the University of Minnesota’s Centre for Infectious Diseases Research and Policy,” sfgate.com reported.
The study has an interesting observation. “Those with mild infections are likely not still infectious by about 10 days after symptoms begin, even if they can still test positive for the virus for days or weeks after symptoms subside,” it said. “This could mean changes in how long hospitals are advised to wait before discharging Covid-19 patients.” The authors wrote: “Based on the present findings, early discharge with ensuing home isolation could be chosen for patients who are beyond day 10 of symptoms with less than 100,000 viral RNA copies per ml of sputum.”
Q: How does the virus attack the body?
A: The virus operates very differently. It starts in the nose before attacking the epithelial cells that line and protect the respiratory tract. When the infection is in the upper airway, patients experience symptoms similar to the common cold. They’ll be contagious but still mobile, still likely to go out in public. “In 10-15% of the moderate cases, the infection slides down the trachea and into the peripheral branches of the lungs, where it attacks two kinds of lung cells — the ones that make mucus, which protects against pathogens and lubricates the airway, and those with hair-like cilia,” Bruce Aylward, an assistant director-general with the WHO was quoted saying. “Cilia cells sweep debris such as pollen or viruses out of the lungs. When they’re killed by an infection, the cilia slough off and fill patients’ airways with fluids and debris.” It is at this stage when some patients develop non-life-threatening pneumonia in both lungs and shortness of breath that the body’s immune cells flood the lungs to clear the organ and repair the damage. In severe cases, however, the body’s response can go overboard, killing not only virus-infected cells but healthy tissue as well, including mucus-producing cells and cilia.
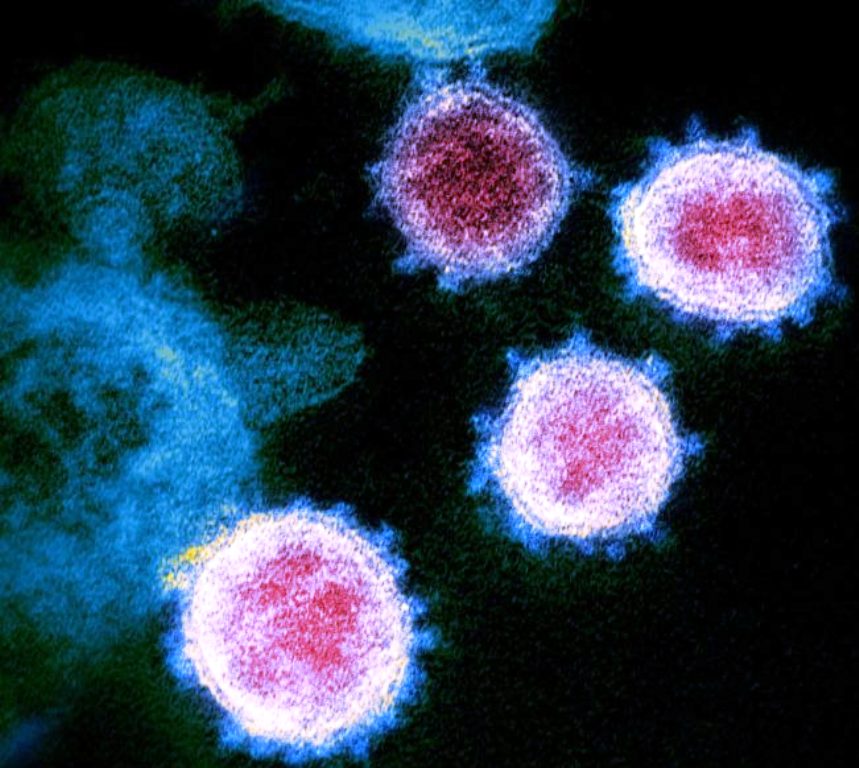
The friendly fire makes pneumonia worse by leaving more debris clogging up the lungs. It is in this stage that situation escalates into severe pneumonia with acute respiratory distress syndrome (ARDS). Those who survive have to live with permanent lung damage including making them vulnerable to bacterial infection. Dr David Morens, senior scientific adviser to the director of the National Institute of Allergy and Infectious Diseases told The Bloomberg: “You pass the tipping point where everything is going downhill and, at some point, you can’t get it back.”
Q: Is there some drug that can be helpful?
A: Many people have made many claims but the scientists have not approved anything so far. Vitamin C supposed to help the immune system is unlikely to help in this case. Western markets witnessed a massive jump in the sales of vitamin C, D, zinc, elderberry supplements, Echinacea herb and many other things. None of these things has been found effective in curing the infection or its shortening.
Recently US president met engineer, industrial designer and science investor, Elon Musk. They shared a feeling that the archaic anti-malaria drug of the 1940s, chloroquine was “maybe worth considering” as a potential treatment. Trump also pointed to another existing drug, Remdesivir, an anti-viral developed by the drug maker Gilead, which is reportedly being used in China to treat COVID-19. This did trigger an interest in pharmaceutical companies about the drug but scientists have not approved anything. US FDA Commissioner Stephen Hahn said while they are working aggressively, it is important “not to provide false hope”.

The Chloroquine is currently being studied at research labs throughout the world. “A group of researchers in France are testing a less toxic derivative of the chloroquine drug called hydroxychloroquine on a few dozen patients with COVID-19, and early reports of the trial indicate that the drug might help shorten the amount of time that people with the disease are infectious,” CNBC reported.
However, “World Health Organization said last month that there is “no proof” the drug is effective in treating the Coronavirus.”
An American biotech company is experimenting with 45 volunteers who got doses of mRNA-1273 into the arms at Kaiser Permanente Washington Research Institute (KPWHRI) last week. The investigational vaccine does not contain any part of the actual Coronavirus and cannot cause infection. Instead, it includes a short segment of lab-grown messenger RNA. Even if all goes well, a vaccine will not be available for widespread use for another 12 to 18 months, according to Anthony Fauci of the US National Institute of Health.
Recently the Westminster gave a £ 2.1million grant to the Oxford University to test if an existing or a new drug helps patients afflicted by the Covid-19. The university has started trials to test the use of the anti-HIV drug along with the anti-malaria drug to treat patients on the basis of the fact that in Australia it was used initially with better success. HIV, it may be recalled here, is also a zoonotic virus.
The Queen’s University in Belfast, according to The Mail got £300,000 to test the 1000 drugs, already in use, on Covid-19 cell to see if any of them is potent enough to control it. Chinese doctors have also used both these drugs in addition to anti-flu Japanese medicine called Favipiravir.
Q: Does any drug accelerate the crisis?
A: Some reports did suggest that people taking anti-inflammatory drugs can have a double impact if infected. Health experts say there is no credible scientific evidence to substantiate the concern that taking ibuprofen, for instance, might worsen the coronavirus infection. WHO said they are collecting the clinical research to find an answer.
The US National Institute of Allergy and Infectious Diseases said “more research is needed to evaluate reports that ibuprofen may affect the course of COVID-19,” but added there is “no evidence that ibuprofen increases the risk of serious complications or of acquiring the virus that causes COVID-19” or other respiratory infections.
Q: What is the quantum of research happening on this disease?
A: Panicked by the crumbling of the economies world over, the countries, charities and the institutions have put in trillions of dollars into the research on the disease. This must be the first virus of history that has triggered so much of funding and research in such a shortest possible time.
There are parallel initiatives going on. IBM, White House and thousands of others have created the largest ever networks of supercomputers to fast-forward the research. Dario Gil, Director of IBM Research told CNN Business that 16 super-computing systems from IBM, national laboratories, several universities, Amazon, Google, Microsoft and others will be provided via remote access to researchers whose projects are approved by the consortium. Using IBM’s Summit supercomputer at the Oak Ridge National Laboratory, the University of Tennessee researchers screened 8,000 compounds to identify the 77 most likely to bind to the main “spike” protein in the coronavirus and render it incapable of attaching to host cells in the human body. In the absence of supercomputer, it would take years to identify the 77 compounds.

Greg Bowman, a professor of biochemistry and molecular biophysics at Washington University in St Louis initiated a project involving crowd-sourcing of computers to create a system of a power of 400 petaflops, with each petaflop having a capacity to carry out one quadrillion calculations per second or three times more powerful than the world’s top supercomputers.
The research is taking place at different levels. While certain institutions are working to evolve a testing kit that can be deployed on a mass scale to reduce the time factor of elaborate testing, some institutions are working to evolve a vaccine. Even some companies specialising in artificial intelligence have also joined in to create some mechanism that will help identify the infected.
Right now, however, only the behaviour of the infection has been elaborately worked on, mostly on the basis of the empirical study involving those who were infected in China, Italy, Iran and other places. The vaccine will take almost a year if scientists succeed in breaking the barrier.
The work as challenging as it is fascinating because the science is working against, what The Washinton Post termed “an evil genius”, that has a zombielike, barely living existence till it lands into the human airway and instantly takes over the control of the host cells.

Dr Muzaffar Jan, a Kashmiri virologist who has the distinction of working under Prof Anthony Fauci, the head of American National Institute of Allergy and Infectious Diseases and is currently a post-doc fellow with Icahn School of Medicine at Mount Sinai, NYC recently wrote that there are multiple challenges that the new virus has thrown up for scientists. “We don’t understand zoonosis or how virus breaks species barrier and spills to into human from wild,” Jan wrote in Kashmir Life. “The viral spike is immunologically silent and developing a vaccine against is tough.” He believes that people who survive the infection may eventually have the answer.
Q: So, how to protect?
A: There is no cure but precaution can help. Avoid getting into crowded places, shaking hands, hugging, and ensure social distancing. Personal hygiene is key to protection and mankind has only one weapon in hand – water and soap, something that is in use for the last 5000 years. Latest research said the soap and water demolish the outer membrane of the virus and makes it literally useless.