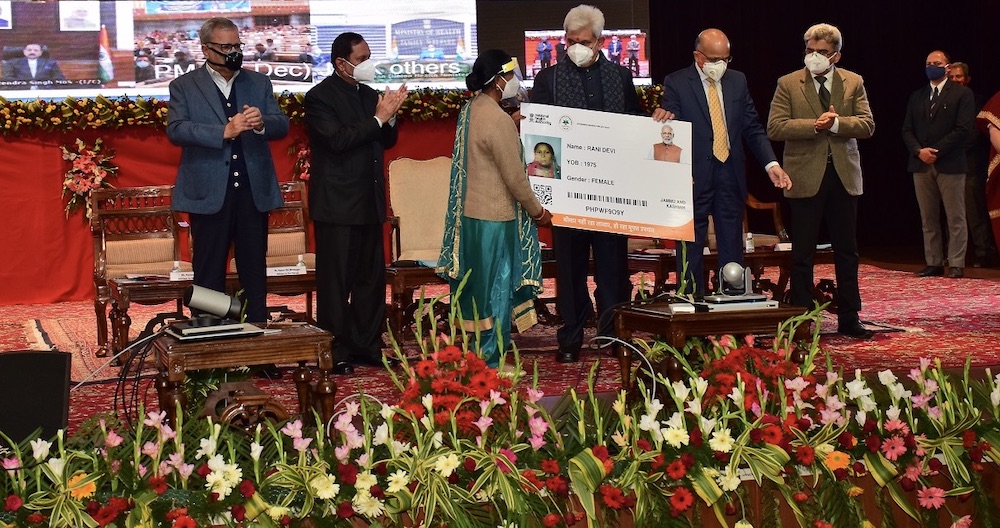
Across Jammu and Kashmir, families long burdened by medical uncertainty are experiencing a quiet transformation, as health-insurance coverage replaces fear with dignity, timely treatment, and the reassurance that illness no longer means financial collapse, Zaid Bin Shabir reports
Barely a month after the wedding festivities ended at Shameema Jan’s home in Srinagar, the family expected life to finally move into some peace. Since 2019, her husband’s work had been irregular, and whatever little they had managed to save had gone into their daughter’s wedding in September 2024.
“Money-wise, we had nothing left, but at least we were at peace that our daughter was married,” her husband said.
One evening, when Shameema’s vision began to blur, she did not pay much attention to it. The same thing had happened earlier in May, and doctors had simply advised her to update her glasses. “I thought it was the same thing again,” she said. “Maybe I was tired after all the wedding work.”
Within days, however, half the vision in her right eye went completely dark. “I could not see anything,” she recalled, lifting her hand to demonstrate. Alarmed, her family rushed her to a private eye hospital in Srinagar.
“We did not think it was something serious,” her daughter said. “We assumed she needed stronger lenses until the doctor advised an MRI.” The reports showed something the family had never imagined. It was a tumour behind her eye that required urgent intervention.
“It felt like someone pulled the floor from under us,” Shameema said. The next morning, the family returned to the hospital seeking clarity. The doctors explained that the treatment would be costly and had to begin immediately, a possibility the family simply could not afford in their circumstances. “We just stared at each other,” her husband said. “We had no money left for even routine check-ups, forget a major procedure.” They felt trapped until a staff member at the hospital asked them if they had the Golden Card. They did not. But they applied immediately and had the card issued within a day.
Within hours, their fear of financial ruin calmed. The treatment they thought they could never afford was carried out without the crushing bills they had been dreading. “The entire procedure was done free of cost,” her husband said. “We had nothing left…nothing. And still, she was treated.”
A year later, Shameema still gets emotional when she talks about it. “First God saved me,” she said. “Then this card did.”

A New Security
Stories like hers are no longer rare. Over the past several years, as more families across Jammu and Kashmir receive and actually use the Golden Card under the Ayushman Bharat Pradhan Mantri Jan Arogya Yojana SEHAT (AB-PMJAY SEHAT), healthcare has started to feel less like a privilege available to only a few. For many households that live month to month, the card has become a safety net against the constant fear of “what if something happens?”
Launched under the National Health Mission at both central and state levels through the National Health Authority (NHA) and the State Health Agencies (SHA). Since 26 December 2020, every resident of Jammu and Kashmir, regardless of income, has been entitled to health coverage of up to Rs 5 lakh per family per year, making it one of the few regions in the country with near-universal insurance. Unlike the rest of India, where it is available to the populations falling below the poverty line, the scheme is implemented for the entire 14 million population in Jammu and Kashmir.
The reach has been extensive. Officials say over 33 lakh Golden Cards have been issued, and with more than 4.5 lakh people treated, the State Health Agency has already paid out hundreds of crores to hospitals. Residents can access benefits at 24,000 empanelled government and private hospitals across India, not just within Jammu and Kashmir.
The scheme is reshaping healthcare-seeking behaviour in Jammu and Kashmir, insiders in the sector assert. A study from GMC Srinagar recorded a sharp rise in complex cardiac procedures after the rollout, indicating that families who had postponed life-saving treatments due to cost are now seeking them on time.
Officials at the Jammu and Kashmir State Health Agency, the body implementing the scheme, said that patients may still fear illness, but they no longer fear financial collapse because of it. Public-health researchers point to a significant drop in out-of-pocket expenses, while policy analysts note that universal eligibility has built a level of trust in government-funded healthcare that did not exist earlier.
Besides, the officials also claimed that the new “trust-based” reimbursement model has streamlined payments to hospitals and improved provider confidence, even as private institutions caution that billing delays and pending dues continue to pose challenges.
“The scheme has shifted Jammu and Kashmir’s healthcare away from a crisis-driven system toward a more predictable, protected and insurance-backed strategy on which families can rely, instead of fear,” a Kashmir-based health official revealed to Kashmir Life.

The Numbers
From its launch in 2020, the scheme expanded across seven policy cycles (PS), each leaving behind a numerical trail that shows how quickly people began depending on it.
In the first policy cycle, PS1, government hospitals issued 17,952 pre-authorisations, while private hospitals generated 31,238, totalling 49,190 interventions worth Rs 17.71 crore. It included Rs 7.01 crore of government and Rs 10.7 crore of private facilities.
The phase saw 49,035 claims submitted–17,806 from government and 31,229 from private hospitals–amounting to Rs 27.18 crore. Of these, 19,950 claims were paid, including 16,869 government and 3,081 private claims, with payouts touching Rs 24.33 crore, while 1,348 claims were rejected, valued at Rs 1.88 crore.
In PS2, numbers dipped slightly as the system stabilised. 18,522 pre-authorisations were issued (6,532 govt, 11,999 private) worth Rs 10 crore. A total of 18,323 claims were submitted (6,376 govt, 11,947 private), amounting to Rs 9 crore, and 17,454 claims were paid, valued at Rs 8 crore. Rejections stood at 856 claims, including 116 private and 740 government, worth Rs 0.88 crore.
| The Golden Card Story | |||||||||
| Claims Submitted (Nos) | Claims Settled (Nos) | Claims Settled (Rs Cr) | |||||||
| Cycle | Private | Public | Total | Private | Public | Total | Private | Public | Total |
| PS1 | 31229 | 17806 | 49035 | 3081 | 16869 | 19950 | 10.08 | 14.25 | 24.33 |
| PS2 | 11947 | 6376 | 18323 | 11824 | 5630 | 17454 | 3.73 | 4.41 | 8 |
| PS3 | 21680 | 8392 | 30072 | 20025 | 5829 | 25854 | 7.29 | 5.04 | 12.33 |
| PS4 | 160.15 | 216.79 | 376.94 | ||||||
| PS5 | 135118 | 237228 | 372346 | 128939 | 213410 | 342429 | 276.59 | 284.79 | 561.38 |
| PS6 | 168884 | 248012 | 416896 | 166190 | 231754 | 397944 | 363.1 | 287.28 | 650.38 |
| PS7 | 124182 | 212677 | 336857 | 68426 | 57597 | 126023 | 155.13 | 73.88 | 229.01 |
| Total | 976.07 | 886.44 | 1862.37 | ||||||
| Source: The Government of Jammu and Kashmir | |||||||||
The PS3 showed a renewed climb. Government hospitals issued 8,996 pre-authorisations and private hospitals 22,504, totalling 31,500 worth Rs 19.25 crore, including Rs 9.24 crore of private hospitals and Rs 10.01 crore of government. Claims submitted reached 30,072 (8,392 govt, 21,608 private), valued at Rs 17.71 crore, while 25,854 claims were paid, totalling Rs 12.33 crore. Rejections included 4,179 claims, worth Rs 4.24 crore.
By the PS4, the scheme scaled aggressively. Insurer paid claims amounting to Rs 376.94 crore.
In PS5, the programme entered a consolidation phase with 3,79,275 pre-authorisations issued—2,42,141 in government hospitals and 1,37,134 in private—worth Rs 696.48 crore. Hospitals submitted 3,72,346 claims, valued at Rs 680.7 crore, while 3,42,429 claims were paid, carrying payouts of Rs 561.38 crore. Rejected claims rose to 37,351, totalling Rs 60.8 crore.
The PS6 marked the scheme’s most dramatic rise, almost transforming it into an essential lifeline for families across the region. Government hospitals issued 2,52,870 pre-authorisations, private hospitals 1,70,438, and together they generated 4,23,308 worth an extraordinary Rs 810.45 crore (Rs 406.02 crore in the government sector, Rs 404.42 crore in the private sector). Claims submitted soared to 4,16,896–2,48,012 in government hospitals and 1,68,884 in private, amounting to Rs 783.33 crore. During this phase, 3,97,944 claims were paid, with payouts reaching Rs 650.38 crore (Rs 287.28 crore government, Rs 363.1 crore private), while 23,844 claims were rejected, valued at Rs 39.04 crore.
The most recent cycle, PS7, reflects both maturity and early signs of correction within the health system. Government hospitals issued 2,24,464 pre-authorisations, while private hospitals issued 1,30,647, totalling 3,57,577, worth Rs 706.02 crore. Hospitals submitted 3,36,857 claims, valued at Rs 639.47 crore, but only 1,26,023 claims were paid—a sharp decline from PS6—amounting to Rs 229.01 crore. Rejections included 3,485 claims, worth Rs 7.17 crore.
Across these seven cycles, the data charts the evolution of a healthcare safety net that expanded far more rapidly than anticipated. From fewer than fifty thousand pre-authorisations in the first cycle to more than four lakh in PS6, and from payouts of Rs 24.33 crore in PS1 to Rs 650.38 crore at their peak, the Golden Card scheme has grown into one of the region’s most widely used social protection programmes.
“It was never just the illness that shook people but the fear of how they would ever afford the treatment,” said a senior official at the State Health Agency (SHA), which implements the AB-PMJAY SEHAT scheme in Jammu and Kashmir. “Earlier, many patients hesitated to even walk into a hospital because they knew it could mean selling land or jewellery. Now, the same families come with confidence. They know they have, in a way, a five lakh rupee health debit card in their pocket.”

The History
The Ayushman Bharat–Pradhan Mantri Jan Arogya Yojana (PMJAY) was introduced in 2018 as one of India’s biggest health protection initiatives, built on a simple idea that no family should be pushed into poverty because someone falls ill. The programme set out to cover over ten crore vulnerable families, nearly fifty crore people, by offering up to Rs 5 lakh per family annually for serious hospitalisation and advanced treatment.
The federally governed Jammu and Kashmir adopted the scheme in December 2018, bringing thousands of households under a safety net they had never experienced before. “The programme has revolutionised the healthcare system in Jammu and Kashmir,” Dr Rahul Sudan, a doctor at GMC Rajouri, told Kashmir Life. “People in far-flung areas have benefited the most. Earlier, if someone needed a hip replacement, the family would worry about arranging lakhs of rupees. Now that fear has ended…you have Rs 5 lakh at your disposal.”
Sudan added that the scheme has eased the burden on long-term dialysis and cancer patients. “We have seen how poor families suffer under the weight of continuous, costly treatments,” he said. “Today, we receive Golden Card beneficiaries from every corner of Jammu and Kashmir, including areas close to the border.”
“When the programme first began here, only families on the Below Poverty Line (BPL) list were eligible,” said another senior SHA official. “But everything changed in December 2020 with the rollout of the SEHAT component. Overnight, every resident of the UT, regardless of income, became entitled to the same coverage.”
Most households in Kashmir fall in the lower-middle or middle-income bracket, he continued, and the region has seen rising cases of kidney failure, long-term dialysis, cancers and other chronic illnesses. “These are conditions that can financially destroy a family,” the official added. “With SEHAT, all of that treatment is covered. The scheme now includes more than 2,000 medical packages, and within India, its impact has been the most transformative in Jammu and Kashmir because this is the only UT where the coverage is universal.”
What Changed
A study published in the European Journal of Cardiovascular Medicine found that after the introduction of the Golden Card scheme, interventional cardiac procedures in Kashmir more than doubled. Angiographies increased from 1661 (2018–2020) to 3858 (2021–2023), angioplasties rose from 1308 to 2103, and advanced device therapies jumped from 24 to 127. Overall, there was a 132 per cent rise in coronary angiographies, a 61 per cent increase in angioplasties, and an 86 per cent jump in pacemaker implantations after the PMJAY launch.
These figures suggest that once financial barriers were removed, patients began seeking earlier and more advanced care that might previously have been postponed. As the study notes, “free of cost and timely delivery of these coronary interventions…ensured better clinical outcomes.”
The authors noted that health insurance was not widely used in Jammu and Kashmir until recently, citing low awareness, socio-cultural factors and the absence of corporate health structures. With the rollout of SEHAT in December 2020, however, the region became universally insured for hospitalisation and major procedures, fundamentally altering access to care.
Another study, published in the Chettinad Health City Medical Journal, assessed 192 hospitalisations across Srinagar, Baramulla, Anantnag and Budgam. It found that 88.5 per cent of patients utilised the scheme, while 11.4 per cent did not. Among the latter, 6.7 per cent faced financial hardship. Although 97.6 per cent of those using the scheme still incurred minor costs, mostly for unavailable medicines or diagnostics, the authors emphasise that the cashless structure significantly reduced the overall burden.
These academic findings mirror the lived experience of families like Naseer Ahmed’s.
Almost two years ago, Naseer Ahmad woke up gasping, chest tight, pain radiating across his ribs. By the time his family gathered around him, he could barely speak. He was stabilised at the District Hospital in Bandipora before being referred to SMHS in Srinagar, nearly 60 kilometres away. There, scans revealed he had lung cancer.
“We just froze,” his brother Parvez recalled. With no stable income, the Rs 5 lakh estimate felt impossible. But when they submitted their Golden Card, already issued under their BPL category, the treatment was processed immediately.
“If we had to pay from our pockets, we simply couldn’t have managed,” Parvez said. “This scheme lifted that weight off us.”
An SHA official noted that the scheme has strengthened government hospitals as well. “When a patient uses, say, Rs 50,000 worth of treatment in a government hospital, that amount is reimbursed. The money returns to the system and is used to upgrade equipment,” the official said, pointing to improvements at SKIMS, JVC, SMHS and the Children’s Hospital.

The Data Explains
The seventh PC data reveals which procedures are most relied upon.
In the private sector, laparoscopic cholecystectomy was the most utilised package, with 20,432 pre-authorisations worth Rs 65 crore reflecting both the prevalence of gallbladder disease and the cost of surgery without support.
Chronic haemodialysis followed with 26,138 sessions (Rs 38.4 crore), and cardiac care remained significant: PTCA with diagnostic angiogram accounted for 1411 cases (Rs 12.6 crore), while PCNL kidney-stone surgery registered 2,639 cases (Rs 10.8 crore). Even haemorrhoidectomy, often delayed due to cost, saw 5517 approvals worth Rs 9.3 crore.
In public hospitals, PTCA with diagnostic angiogram again topped utilisation, with 2,031 cases worth Rs 18.2 crore. Unspecified surgical packages (1,075 cases; Rs16.3 crore) highlighted the unpredictability of emergency care. Severe sepsis accounted for 7,681 hospitalisations (Rs12.7 crore), while the Special Neonatal Care Package treated 6,432 infants (Rs12.7 crore). Laparoscopic cholecystectomy remained among the top procedures with 4,790 cases worth Rs11.3 crore.
Misra Begum’s story underscores what these numbers mean in real life. Ten years after losing her young son to a sudden brain haemorrhage, Misra, 65, lived quietly with her ailing husband in Srinagar’s Nowshera. Last summer, severe abdominal pain brought her to SKIMS, where doctors diagnosed her with intestinal cancer.
“When the doctor said it, I felt like I left my body,” she recalled. Her husband was prepared to borrow money until they learned the surgery would be covered under the Golden Card, aside from a few small purchases.
“Schemes like this were hardly meant for people like us,” she said. Her treatment continues, but she never fell into debt. “If the card hadn’t been there, I don’t think I would be alive today.”
The Worries
The scheme, however, hasn’t been free of concerns. “As the scheme grew, so did the triggers. We began noticing patterns that didn’t feel right,” the official said. “Some private hospitals were found indulging in questionable practices, especially in gallbladder surgeries and even maternity care. There were instances where women who were medically fit for normal delivery were allegedly pushed into unnecessary C-sections, only to inflate claim amounts.”
To strengthen the State Anti-Fraud Unit (SAFU), SHA suspended five private hospitals for suspicious activities and imposed penalties of Rs 29,62,000 on several others. Over 12,000 triggers forwarded by NAFU were audited, uncovering 450 cases of abuse or fraud and leading to the rejection of claims worth Rs 1,04,62,350.
Fraud was not the only challenge. A major hurdle emerged last year when IFFCO Tokio General Insurance Company (GIC), the insurer responsible for implementing the Golden Card scheme, issued an exit notice, plunging the programme into legal uncertainty. It said it is losing money as the premium of Rs 1840 per family is not offering it enough income against a disproportionate outgo. They replaced the Bajaj Allianz, the insurer that managed the scheme for two initial years at a premium of Rs 849 per family and exited in the wake of surging losses.
Following the exit notice, the SHA, on the advice of the Department of Law, Justice and Parliamentary Affairs, applied Section 37 of the Arbitration and Conciliation Act, 1996, challenging a High Court order of February 2, 2024.
On March 7, 2024, the High Court directed both parties to maintain the status quo March 11, 2024, a direction was issued that was extended multiple times. Despite this, IFFCO Tokio discontinued the scheme beyond March 14, 2024, leaving thousands of patients and hospitals in limbo.
A judgment delivered on August 28, 2024, disposed of the petition but directed IFFCO Tokio to temporarily continue operations under the existing contract until an arbitrator resolves the dispute. In response, the company filed another appeal against the order.
“There are three modes of implementation,” an SHA official explained. “The first is the insurance model, where the State Health Agency hires an insurance company and pays them based on the targeted families. The second is the trust mode, where the SHA handles everything, from processing claims to making payments. The third is a mixed mode.”
“Right now, we are operating entirely in trust mode,” he added. “After the insurance company exited, we took over the whole system and now manage every aspect ourselves.” The SHA has removed a set of surgical procedures, which were making the bulk of the claims from public as well as the private sector hospitals. This has removed the outgoing burden of the agency, a society registered under the law.
For all its flaws, delays and disputes, the Golden Card has altered something fundamental in Kashmir’s relationship with illness. “It did not just fund treatments, but it also restored a sense of security that life-threatening illnesses had stolen from countless homes across Jammu and Kashmir,” said Dr Shah, a former general physician at GMC Baramulla.
Names of some patients have been changed at their request.